Elimination of Routine Screening Laboratory Tests for Psychiatric Admission: A Quality Improvement Initiative
Abstract
Objective:
Research has shown that routine screening laboratory tests for patients with mental health symptoms admitted to psychiatry units find little unexpected clinical abnormalities. This study examined the effects on cost of care and patient safety measures of a hospital change in policy in which such routine tests were no longer required.
Methods:
This retrospective cohort study analyzed data from all patients admitted from the emergency department (ED) to inpatient psychiatry at a tertiary care hospital 4 months before and 4 months after the policy change. Primary outcome measures were number and costs of laboratory tests ordered in the ED and during the inpatient stay. Secondary measures included length of stay (LOS) and number of hospital consultations during admission, patient transfers to nonpsychiatry services, and inpatient deaths. Chi-square tests and Wilcoxon rank sum tests were used to examine group differences.
Results:
In total, data from 1,910 patients were included (886 preimplementation and 1,024 postimplementation). The median number of lab tests ordered during the hospital stay decreased from three (interquartile range [IQR]=3) to two (IQR=3). The median total lab charges decreased from $445 (IQR=$291) to $312 (IQR=$497). Mean ED LOS decreased by 5.5 hours, and the proportion of patients with no blood lab orders increased from 22% to 40%. No increases in consultations or transfers were noted. No patients died at any point.
Conclusions:
A policy that avoids routine laboratory screening tests for patients admitted to inpatient psychiatry can save money, improve patient care, and decrease LOS, without increasing adverse outcomes.
HIGHLIGHTS
Routine screening lab tests are frequently used to help ensure no acute medical pathology is present before inpatient psychiatric admission.
An institutional policy to eliminate routine lab tests at a large tertiary care hospital decreased costs and reduced length of stay in the emergency department and hospital.
Adverse events showed no increase among admitted patients after the policy change.
It is estimated that in 2017, 46.6 million adults were living with mental illness in the United States (1). Persons with mental illness frequently seek care in the emergency department (ED), with estimates indicating that one in eight ED visits are directly or indirectly related to mental health (2). According to the National Hospital Ambulatory Medical Care Survey, 5.485 million ED visits in 2016 were for a primary psychiatric diagnosis (3). The ED provider has several objectives when evaluating these patients: initially stabilizing the patient if unsafe behaviors exist, assessing whether a medical pathology could be playing a role in the presenting symptoms, determining disposition to either inpatient admission or discharge from the ED, and determining the appropriate admitting service (psychiatry vs. hospital medicine).
Historically, assessment for medical pathology as a cause of the presenting symptoms or complaints has been referred to as “medical clearance” and typically involves routine ordering of a set of laboratory tests (4, 5). The intention of ordering these blood and urine tests is to screen for clinical abnormalities that could be contributing to a patient’s symptoms and to assist the ED physician in determining the appropriate admitting service. The specific laboratory tests that are routinely required vary widely among practices and hospitals.
There has been debate about the benefits of routine screening labs. Although the literature suggests some utility of this practice (6–14), most recent studies have shown that the vast majority of abnormalities detected by laboratory tests were for patients for whom a test was ordered after a clinical history review or physical exam. These studies concluded that ordering routine screening laboratory tests has little to no value (15–26). Other studies have reported utility of more nuanced ordering of screening labs for certain patient populations, such as elderly persons and patients with no previous psychiatric history (27–29). Ultimately, several position statements from professional groups (e.g., the American College of Emergency Physicians and American Association for Emergency Psychiatry) have spoken out against ordering routine lab tests (30–32). Although this position is generally strongly supported by emergency medicine practitioners, the psychiatry community has been much slower in endorsing it (33). Most hospitals still have guidelines that require mandatory screening lab tests for psychiatric admission (34).
In 2018, a communitywide collaborative among emergency medicine and psychiatry leaders, supported by the Institute for Clinical Systems Improvement, was convened. This group evaluated the evidence and position statements regarding routine screening laboratory testing, shared individual institutional policies regarding this practice, and agreed to a change in local community practice whereby patients being admitted to the inpatient psychiatry service had lab tests ordered “based on individual patient history and exam” (35). The aim of the study reported here was to evaluate the effects of eliminating the requirement for routine screening lab tests for patients admitted to the psychiatric service.
Methods
Study Setting and Participants
This study was conducted at a large tertiary care hospital with a 100-bed adult inpatient psychiatric unit. All pediatric and geriatric patients needing psychiatric admission are transferred elsewhere. Approximately 88,000 patients per year arrive in our ED, of whom roughly 3,500 are admitted to the inpatient psychiatry service. Within the ED, an 11-room care area is dedicated for patients with mental health complaints, staffed by emergency physicians, physician assistants, residents, and social workers. On April 16, 2018, a change in policy was made from routine ordering of laboratory tests to ordering based on individual patient evaluations. Data were obtained for a 4-month period before the change (December 15, 2017–April 15, 2018) and a 4-month period starting 1 month after the change (May 16–September 16, 2018). This allowed 1 month for the new process to become routine practice, allowing for more representative data.
Data from all patients admitted from the ED to the inpatient psychiatric service were included. This cohort included those who arrived with a clear primary mental health complaint, as well as those who may have been initially seen for injuries, ingestions, drug use, alcohol intoxication, or medical symptoms and who were eventually medically cleared and found to meet criteria for psychiatric admission.
This project was reviewed by the Regions Hospital Institutional Review Board (IRB), which judged it to be a quality improvement project and not to require ongoing IRB oversight.
Interventions
Before the change in policy, the hospital’s standard admission order set required for inpatient psychiatric admission included orders for complete blood count (CBC), basic metabolic panel, urinalysis, basic urine drug screen, and urine pregnancy test when applicable. After the policy change, these lab tests were no longer required and were ordered at the discretion of the ED provider or at the request of the admitting psychiatric service.
Measurements
All data elements for this study were retrospectively obtained from electronic medical record data, and billing and coding data were retrieved via an automated data query. The data sets were created by hospital analysts who were blinded to the study hypothesis. Data included patient demographic characteristics, arrival information, diagnoses, common medical comorbid conditions, and common lab orders, as well as orders for electrocardiograms or noncontrast computed tomography head scans. Costs for lab and other diagnostic tests were determined according to the charge master of the hospital during the study period. We also collected orders for consultations and patient transfers to hospital medicine service or the intensive care unit (ICU) service. Finally, we collected ED and inpatient length of stay (LOS).
Outcomes
The primary outcomes for this evaluation were the total number of lab tests ordered and total charges for these orders. The charged orders included any placed from patient arrival in the ED to patient discharge from the hospital. Secondary outcomes included the number of lab tests ordered during the ED and inpatient stays, cost of tests ordered during the ED and inpatient stays, ED and hospital LOSs, inpatient consultations for hospital medicine or specialty services, transfer to hospital medicine, transfer to ICU, and death.
Analysis
Analyses were performed with SAS software, version 9.4. Descriptive statistics, including frequency, means and SDs, and medians and interquartile ranges (IQRs), were generated as appropriate for variables of interest. Because the data were nonnormally distributed, all continuous variables were described by median and IQR, except when this was not informative (i.e., a median of 0; see below). Chi-square tests were used to statistically assess differences among categorical variables between the pre and post groups. For continuous variables, Wilcoxon rank sum tests were used to compare the pre and post groups with a 95% confidence level. For a given individual lab test, we determined whether it was ordered for a patient. For total cost analysis, we included all lab tests ordered, including multiples of the same test if applicable. For example, a patient who was admitted with slight anemia that was monitored with several CBC orders over several days to assess for stability would be counted as a single order for CBC in the lab order analysis but as multiple lab orders in the cost and total labs analysis. We chose this analysis to avoid any skewing that would happen because of inpatients with multiple similar lab orders during their stays.
Results
Data from 1,910 patients were included in the analysis (886 in the preimplementation cohort and 1,024 in the postimplementation cohort), of whom 1,028 (54%) were male. Patient characteristics are shown in Table 1. Patients in the postimplementation cohort were slightly older and had a higher incidence of coronary artery disease and hypertension as comorbid conditions, but these differences were not clinically relevant. The two groups did not clinically significantly differ in admitting diagnoses. All other demographic variables were balanced between the two groups.
| Policy implementation group | |||||
|---|---|---|---|---|---|
| Pre (N=886) | Post (N=1,024) | ||||
| Characteristic | N or median | % or IQR | N or median | % or IQR | p |
| Age in years (median, IQR) | 34 | 20 | 35 | 22 | .014 |
| Gender | .052 | ||||
| Male | 498 | 56 | 530 | 52 | |
| Female | 388 | 44 | 494 | 48 | |
| Race-ethnicity | .916 | ||||
| White | 573 | 65 | 675 | 66 | |
| Black or African American | 180 | 20 | 210 | 21 | |
| Asian | 51 | 6 | 46 | 4 | |
| Hispanic or Latino | 31 | 4 | 42 | 4 | |
| American Indian or Alaska Native | 14 | 2 | 13 | 1 | |
| Native Hawaiian or Pacific Islander | 5 | 1 | 3 | <1 | |
| Other or unknown | 20 | 2 | 22 | 2 | |
| Triage acuity levelb | .421 | ||||
| 1 | 2 | <1 | 2 | <1 | |
| 2 | 821 | 93 | 952 | 93 | |
| 3 | 56 | 6 | 68 | 7 | |
| 4 | 6 | 1 | 2 | <1 | |
| 5 | 1 | <1 | 0 | — | |
| Arrival in ED | .780 | ||||
| Ambulance | 214 | 32 | 304 | 32 | |
| Car | 203 | 31 | 295 | 31 | |
| Police | 63 | 10 | 98 | 10 | |
| Walk-in | 22 | 3 | 33 | 4 | |
| Public transport or taxi | 36 | 4 | 44 | 4 | |
| Other or unknown | 12 | 14 | 166 | 16 | |
| Time of day of ED arrivalc | .916 | ||||
| Day | 372 | 42 | 424 | 41 | |
| Evening | 384 | 43 | 443 | 43 | |
| Night | 130 | 15 | 157 | 15 | |
| Vital signs (median, IQR) | |||||
| Systolic blood pressure | 124 | 24 | 123 | 36 | .832 |
| Diastolic blood pressure | 76 | 19 | 74 | 20 | .040 |
| Heart rate | 75 | 30 | 74 | 28 | .418 |
| Comorbid condition | |||||
| Diabetes | 62 | 7 | 95 | 9 | .071 |
| Heart disease | 15 | 2 | 40 | 4 | .004 |
| Hypertension | 140 | 16 | 197 | 19 | .049 |
| Kidney disease | 12 | 1 | 14 | 1 | .981 |
| Admitting diagnosis group (ICD-10 code) | .023 | ||||
| Substance abuse disorder (F10.0–F19.99) | 63 | 7 | 99 | 10 | |
| Psychotic disorder (F20.0–F29.99) | 319 | 36 | 321 | 31 | |
| Mood disorder (F30.0–F39.99) | 319 | 36 | 407 | 40 | |
| Other (F40.0 or above) | 181 | 21 | 188 | 19 | |
TABLE 1. Characteristics of patients admitted from a hospital emergency department (ED) to its inpatient psychiatry unit, by groupa
Primary Outcome
Because the number of lab tests and hospital charges were not normally distributed, results are presented as medians with IQRs (Table 2). The median number of total lab tests ordered in the ED pre- to postimplementation decreased from three to one (p<0.001). The median number of lab tests ordered in the hospital was identical between the two groups (0), likely because no tests were ordered for a large number of patients, skewing the data toward the median of zero. The mean±SD number of lab tests ordered in the hospital, however, increased from pre- to postimplementation, from 0.94±3.00 to 1.47±2.81 (p<0.001). The total median number of tests ordered during the hospital stay (ED arrival to hospital discharge) decreased from three to two (p<0.001).
| Policy implementation group | |||||
|---|---|---|---|---|---|
| Pre (N=886) | Post (N=1,024) | ||||
| Characteristic | N | % | N | % | p |
| Blood lab orders | |||||
| Complete blood count | |||||
| ED | 621 | 70 | 255 | 25 | <.001 |
| Inpatient | 100 | 11 | 291 | 28 | <.001 |
| Chemistry panel | |||||
| ED | 636 | 72 | 309 | 30 | <.001 |
| Inpatient | 119 | 13 | 291 | 28 | <.001 |
| Liver enzymes | |||||
| ED | 76 | 9 | 75 | 7 | .311 |
| Inpatient | 171 | 19 | 226 | 22 | .137 |
| Lipase | |||||
| ED | 14 | 2 | 8 | 1 | .103 |
| Inpatient | 11 | 1 | 11 | 1 | .733 |
| Ethanol | |||||
| ED | 41 | 5 | 51 | 5 | .719 |
| Inpatient | 0 | — | 3 | <1 | .107 |
| Magnesium | |||||
| ED | 13 | 1 | 17 | 2 | .735 |
| Inpatient | 63 | 7 | 73 | 7 | .988 |
| Troponin | |||||
| ED | 11 | 1 | 19 | 2 | .282 |
| Inpatient | 18 | 2 | 21 | 2 | .976 |
| Urine lab orders | |||||
| Urine drug test | |||||
| ED | 560 | 63 | 551 | 54 | <.001 |
| Inpatient | 28 | 3 | 101 | 10 | <.001 |
| Urinalysis | |||||
| ED | 242 | 27 | 156 | 15 | <.001 |
| Inpatient | 40 | 5 | 63 | 6 | .114 |
| Urine pregnancy test | |||||
| ED | 121 | 14 | 116 | 11 | .124 |
| Inpatient | 22 | 2 | 42 | 4 | .050 |
| Total lab orders | Median | IQR | Median | IQR | p |
| Total blood lab tests | |||||
| ED | 2 | 2 | 0 | 2 | <.001 |
| Inpatient | 0 | 1 | 0 | 2 | <.001 |
| Total | 2 | 2 | 2 | 3 | <.001 |
| Total labs | |||||
| ED | 3 | 2 | 1 | 3 | <.001 |
| Inpatient labs | 0 | 1 | 0 | 2 | <.001 |
| Total | 3 | 3 | 2 | 3 | <.001 |
| Charges | |||||
| Total lab charges ($) | |||||
| ED | 405 | 306 | 93 | 312 | <.001 |
| Inpatient | 0 | 198 | 0 | 312 | <.001 |
| Total | 445 | 291 | 312 | 497 | <.001 |
| Other orders | N | % | N | % | |
| CT scan head | |||||
| ED | 21 | 2 | 22 | 2 | .745 |
| Inpatient | 47 | 5 | 34 | 3 | .032 |
| Electrocardiogram | |||||
| ED | 116 | 13 | 135 | 13 | .953 |
| Inpatient | 168 | 19 | 194 | 19 | .993 |
| Length of stay (M±SD) | |||||
| ED (minutes) | 810±926 | 478±651 | <.001 | ||
| Inpatient (hours) | 114±194 | 98±136 | .003 | ||
| Consultations, transfers, deaths | |||||
| Hospital medicine consultations | 171 | 19 | 206 | 20 | .655 |
| Other consultations | 29 | 3 | 38 | 4 | .604 |
| Transfer to hospital medicine | 8 | 1 | 13 | 1 | .444 |
| Transfer to intensive care unit | 0 | — | 0 | — | |
| Death | 0 | — | 0 | — | |
TABLE 2. Characteristics of orders for laboratory tests, charges for tests, and outcomes for patients admitted from a hospital emergency department (ED) to its inpatient psychiatry unit, by groupa
The daily median number of lab orders during hospitalization are shown in Figures 1, 2, and 3. The number of patients with no lab tests ordered at any point during the hospital stay increased from 82 (9%) to 206 (20%) (p<0.001). The number of patients with no tests requiring a blood draw increased from 194 (22%) to 411 (40%) (p<0.001).
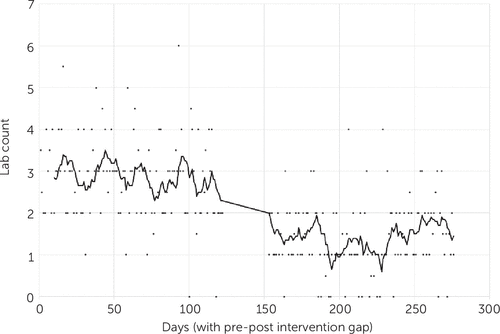
FIGURE 1. Total median number of laboratory tests (lab counts) ordered each day for patients who were in the emergency departmenta
aData were obtained for 4 months before the end of a policy requiring routine lab tests for psychiatric admissions (December 15, 2017–April 15, 2018; days 1–122) and for 4 months starting 1 month after that change (May 16–September 16, 2018; days 152–276).
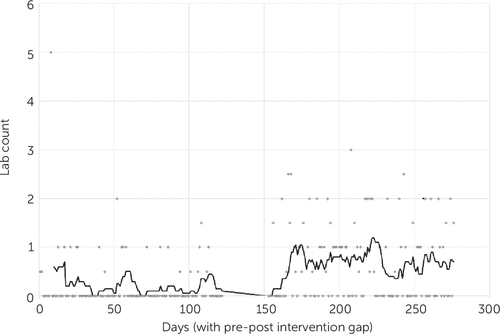
FIGURE 2. Total median number of laboratory tests (lab counts) ordered each day for patients during inpatient hospitalizationa
aData were obtained for 4 months before the end of a policy requiring routine lab tests for psychiatric admissions (December 15, 2017–April 15, 2018; days 1–122) and for 4 months starting 1 month after that change (May 16–September 16, 2018; days 152–276).
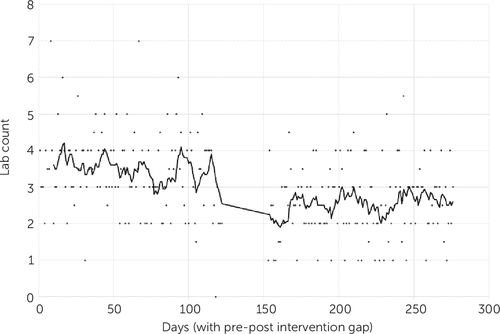
FIGURE 3. Total median number of laboratory tests (lab counts) ordered each day from patients’ arrival in the emergency department to hospital dischargea
aData were obtained for 4 months before the end of a policy requiring routine lab tests for psychiatric admissions (December 15, 2017–April 15, 2018; days 1–122) and for 4 months starting 1 month after that change (May 16–September 16, 2018; days 152–276).
The most notable pre- to postimplementation decreases in specific lab orders in the ED included the CBC (70% to 25%, p<0.001), chemistry panel (72% to 30%, p<0.001), urinalysis (27% to 15%, p<0.001), and urine drug screen (63% to 54%, p<0.001). The ordering of most of these tests increased in the inpatient psychiatry unit, except for the urinalysis, which did not change significantly.
The total median ED lab charges per patient decreased from $405 to $93 (p<0.001). The total median inpatient lab charges were $0 before and after the change, and the total mean inpatient lab charges per patient increased from $139.59±$447.81 to $212.78±$400.91 (p<0.001). The median total lab charges per patient during the hospital stay (ED arrival to hospital discharge) decreased from $445 to $312 (p<0.001), representing a cost saving of $133 per patient. When multiplied by our postintervention patient cohort of 1,024 patients, this represents total savings of $136,192.
The mean LOS in the ED decreased from 810.0 to 477.5 minutes (p<0.001), and the mean LOS in the hospital from 113.9 to 97.9 hours (p=0.003). The percentage of consultations placed by the psychiatry service for inpatient medical or other consultation services did not change after the policy change. There were 171 consultations (19%) for inpatient medicine before the change and 206 consultations (20%) after the change. Moreover, no change was detected in the percentage of consultations with other services, with 29 (3%) consultations before and 38 (4%) after the policy change. The number of patients transferred to the hospital medicine service was 8 (1%) before the change and 13 (1%) after it. No patients in either cohort were transferred to the ICU or died during the hospital stay.
Discussion
The psychiatry community has historically been reluctant to substantially change the practice of requiring routine screening lab tests for psychiatric admission. The reasons for this are likely multifactorial. The clinical presentation of possible mental health crises can mimic many other medical emergencies. Inpatient psychiatric hospitals typically have fewer resources to care for patients with acute medical conditions. Likewise, psychiatrists have limited training and experience caring for nonpsychiatric illnesses. Arguments against the indiscriminate ordering of routine lab tests do not deny their utility. Rather, the focus is on placing orders for appropriately selected patients—those with abnormal vital signs, abnormal findings on a physical exam, or concerns raised after review of the patient’s medical history.
To our knowledge, this is the first evaluation of a real-world change in practice in which routine lab orders are no longer required for admitted psychiatry patients. We observed a number of benefits without any obvious deleterious effects. These benefits included fewer blood tests, which equated to fewer blood draws, as evidenced by the increased number of patients with no blood lab orders; lower cost of care; and decreased LOS in both the ED and the hospital. Together, these improvements represent the three dimensions of the “triple aim” of the Institute for Healthcare Improvement (36). Another patient-centered benefit of not utilizing routine screening labs before admission is a reduced risk for escalating agitation by forcing a patient to undergo an invasive blood draw. This reduces the risk of harm to the patient and the care team and has the potential to improve ED throughput of patients. Finally, the decrease in urinalysis ordering may have led to fewer false-positive diagnoses of urinary tract infections and fewer antibiotic prescriptions.
The large decrease in lab ordering in the ED was somewhat offset by a less pronounced increase in lab ordering of nearly all the same lab tests during the inpatient stay. However, the total overall lab ordering decreased significantly. Perhaps most important, the percentage of patients with no lab orders increased from 9% to 20%, and the proportion of patients with no blood lab orders increased from 22% to 40%. In our cohort, this represents a substantial number of patients who did not have to undergo invasive and painful needle pokes.
The least pronounced decrease in lab ordering was the order for a urine drug screen. This could suggest a utility of this test—perhaps to help with evaluating specific symptoms or to help with disposition of patients with possible chemical dependence. Ordering of other tests, such as liver panel, troponin level, and alcohol level, was similar before and after the policy change both in the ED and the inpatient ward. This similarity suggests that the policy change did not necessarily affect the ordering of tests that were tailored more specifically to individual patients.
The decreased LOS in the ED was to be expected, given a decrease in time spent waiting for lab samples to be obtained from the patient and processed in the lab. Of note, inpatient LOS also decreased. These decreases in LOS certainly translated to improved timeliness of patient care. Increased throughput indicates increased capacity to care for patients, which likely translated to decreased cost for individual patients and possibly increased revenue for the hospital.
Of note, lab tests ordered in the ED were at the discretion of the provider. However, the accepting psychiatry provider could request specific lab tests before accepting the patient. This collaborative aspect of patient care did not change after the policy change.
Several factors may explain why the rate of lab ordering for the required admission lab tests (CBC, chemistry panel, urinalysis, urine pregnancy test, and urine drug screen) before the policy change was not 100%, as might be expected when these tests were part of the routine order set. If patients had tests ordered within the 6 months before admission, repeat lab test orders were not required. If a patient could not urinate before being transferred to inpatient care, the urinalysis, urine pregnancy test, and urine drug screen were deferred to inpatient care. In addition, patients frequently refuse lab tests, which, if deemed that the results are unlikely to be abnormal, are also often deferred to inpatient care.
A strength of the study was that it was a simple before-and-after study at a single institution. During the study period, no other major policy changes were implemented that would likely have affected the outcomes examined here. This provided a unique opportunity to evaluate behavior change in a straightforward manner. Second, all the data were obtained through automated retrieval from an administrative database. Because of this, the study could be completed in a timely manner, with little risk for introducing bias into the data abstraction process. The data set included a large number of patients over a 9-month period, allowing inclusion of patients with a multitude of psychiatric diagnoses. Finally, although this was a retrospective review, the data set was robust. It was generated by several analysts with routine experience in conducting similar electronic medical record queries.
Previously, hospitals have been reluctant to adopt the policy change that we have described here. With the current findings supporting these changes, perhaps more hospitals can move from one-size-fits-all policies to more nuanced policies of tailored lab ordering.
Some limitations of this study should be noted. A notable limitation was that the study was conducted at a busy tertiary care center, with extensive experience caring for patients with mental illness and a large psychiatry inpatient unit. Moreover, experienced emergency physicians, physician assistants, and social workers examined these patients. These factors may limit the generalizability to other facilities with fewer resources. Additionally, it is possible that patients undergoing routine screening labs in the cohort before the policy change would have had notable lab test abnormalities that precluded their admission to the psychiatry service. In theory, this would have led to a more carefully screened patient group and would have led to fewer transfers to the hospital medicine service during that period. Because this outcome was not observed, it is unlikely that this scenario affected the composition of our patient cohort.
Previous research has shown a reduction in test ordering after various initiatives; however, sustainability of the reduced ordering has not been studied as thoroughly (37). Future investigations could evaluate whether similar policy changes lead to enduring changes in practice. The policy change described here included all patients admitted to inpatient psychiatry, regardless of age, comorbid conditions, and diagnoses. We did not evaluate the utility of lab ordering in specific patient subgroups; future research and policy changes may consider explicit recommendations for higher-risk patient groups, such as older patients or patients with substance use disorders.
Conclusions
A change in policy to no longer routinely requiring screening lab tests for patients admitted to the inpatient psychiatry unit resulted in fewer tests ordered and median cost savings of $133 per patient or $136,192 across the postintervention cohort of patients. The number of lab tests requiring blood draws also significantly decreased, as did patients’ LOS. This was achieved without any notable adverse outcomes, such as increased hospital consultations or increased rates of transfer from psychiatry to hospital medicine or the ICU. No deaths occurred among any patients in this study. Adoption of a similar policy by other hospitals may improve patient care and reduce cost.
1 Mental Health Information: Statistics. Bethesda, MD, National Institute of Mental Health, 2019. https://www.nimh.nih.gov/health/statistics/mental-illness.shtml. Accessed Aug 14, 2019Google Scholar
2 Owens PL, Mutter R, Stocks C: Mental Health and Substance Abuse–Related Emergency Department Visits Among Adults, 2007. HCUP Statistical Brief 92. Rockville, MD, Agency for Healthcare Research and Quality, Healthcare Cost and Utilization Project, 2010. https://www.hcup-us.ahrq.gov/reports/statbriefs/sb92.pdf. Accessed Aug 14, 2019Google Scholar
3 National Hospital Ambulatory Medical Care Survey: 2016 Emergency Department Summary Tables. Hyattsville, MD, Centers for Disease Control, National Center for Health Statistics, 2016. https://www.cdc.gov/nchs/data/nhamcs/web_tables/2016_ed_web_tables.pdf. Accessed Aug 14, 2019Google Scholar
4 : Emergency department medical clearance of patients with psychiatric or behavioral emergencies: part 1. Psychiatr Clin North Am 2017; 40:411–423Crossref, Medline, Google Scholar
5 : Emergency department medical clearance of patients with psychiatric or behavioral emergencies, part 2: special psychiatric populations and considerations. Psychiatr Clin North Am 2017; 40:425–433Crossref, Medline, Google Scholar
6 : Admissions screening: clinical benefits. Ann Intern Med 1975; 83:197–203Crossref, Medline, Google Scholar
7 : Physical illness presenting as psychiatric disease. Arch Gen Psychiatry 1978; 35:1315–1320Crossref, Medline, Google Scholar
8 : Unrecognized physical illness prompting psychiatric admission: a prospective study. Am J Psychiatry 1981; 138:629–635Link, Google Scholar
9 : Morbidity and rate of undiagnosed physical illnesses in a psychiatric clinic population. Arch Gen Psychiatry 1979; 36:414–419Crossref, Medline, Google Scholar
10 : The psychiatric physical examination: part II. findings in 75 unselected psychiatric patients. J Clin Psychiatry 1981; 42:99–102Medline, Google Scholar
11 : Physical disorders among emergency psychiatric patients. Can J Psychiatry 1981; 26:65–67Crossref, Medline, Google Scholar
12 : Prospective evaluation of emergency department medical clearance. Ann Emerg Med 1994; 24:672–677Crossref, Medline, Google Scholar
13 : Screening CMHC outpatients for physical illness. Hosp Community Psychiatry 1990; 41:786–790Abstract, Google Scholar
14 : A tool for the emergency medicine evaluation of psychiatric patients. Am J Emerg Med 1996; 14:329–333Crossref, Medline, Google Scholar
15 : Medical clearance and screening of psychiatric patients in the emergency department. Acad Emerg Med 1997; 4:124–128Crossref, Medline, Google Scholar
16 : Emergency medical evaluation of psychiatric patients. Ann Emerg Med 1994; 23:859–862Crossref, Medline, Google Scholar
17 : Routine laboratory testing for medical disorders in psychiatric inpatients. Arch Intern Med 1985; 145:2085–2088Crossref, Medline, Google Scholar
18 : “Medical clearance” of psychiatric patients without medical complaints in the emergency department. J Emerg Med 2000; 18:173–176Crossref, Medline, Google Scholar
19 : Routine laboratory testing to evaluate for medical illness in psychiatric patients in the emergency department is largely unrevealing. West J Emerg Med 2009; 10:97–100Medline, Google Scholar
20 : A retrospective review of screening labs for medical clearance in a military population. Mil Med 2015; 180:1128–1131Crossref, Medline, Google Scholar
21 : Protocolized laboratory screening for the medical clearance of psychiatric patients in the emergency department: a systematic review. Acad Emerg Med 2018; 25:566–576Crossref, Medline, Google Scholar
22 : Effects of mandatory screening labs in directing the disposition of the apparently healthy psychiatric patient in the emergency department. US Army Med Dep J 2017; July–Sept:18–24Google Scholar
23 : Role of urine drug screening in the medical clearance of pediatric psychiatric patients: is there one? Pediatr Emerg Care 2013; 29:903–906Crossref, Medline, Google Scholar
24 : Clinical utility of screening laboratory tests in pediatric psychiatric patients presenting to the emergency department for medical clearance. Ann Emerg Med 2014; 63:666–75.e3Crossref, Medline, Google Scholar
25 : Is medical clearance necessary for pediatric psychiatric patients? J Emerg Med 2014; 46:800–807Crossref, Medline, Google Scholar
26 : Psychiatric patients in the pediatric emergency department undergoing routine urine toxicology screens for medical clearance: results and use. Pediatr Emerg Care 2009; 25:387–392Crossref, Medline, Google Scholar
27 : Medical screening of mental health patients in the emergency department: a systematic review. J Emerg Med 2018; 55:799–812Crossref, Medline, Google Scholar
28 : A screening tool to medically clear psychiatric patients in the emergency department. J Emerg Med 2012; 43:871–875Crossref, Medline, Google Scholar
29 : Medical screening in the emergency department for psychiatric admissions: a procedural analysis. Gen Hosp Psychiatry 2004; 26:405–410Crossref, Medline, Google Scholar
30 Clinical Policy: Critical Issues in the Diagnosis and Management of the Adult Psychiatric Patient in the Emergency Department (2017). Irving, TX, American College of Emergency Physicians, 2017. https://www.acep.org/patient-care/clinical-policies/Psychiatric-Patient. Accessed Aug 14, 2019Google Scholar
31 : American Association for Emergency Psychiatry Task Force on Medical Clearance of Adults part I: introduction, review and evidence-based guidelines. West J Emerg Med 2017; 18:235–242Crossref, Medline, Google Scholar
32 : American Association for Emergency Psychiatry Task Force on Medical Clearance of Adult Psychiatric Patients. Part II: controversies over medical assessment, and consensus recommendations. West J Emerg Med 2017; 18:640–646Crossref, Medline, Google Scholar
33 American Psychiatric Association Practice Guidelines for the Psychiatric Evaluation of Adults, 3d ed. Arlington, VA, American Psychiatric Association, 2016.Google Scholar
34 : ED utilization of medical clearance testing for psychiatric admission: National Hospital Ambulatory Medical Care Survey analysis. Am J Emerg Med 2018; 36:745–748Crossref, Medline, Google Scholar
35 Summary: Medical Clearance Evaluation in the ED for People With Mental Health Needs. Bloomington, MN, Institute for Clinical Systems Improvement, Minnesota Health Collaborative: Mental Health, 2019. https://www.icsi.org/wp-content/uploads/2019/10/Medical-Clearance-in-the-ED-Summary-10.15.19-FINAL-4.pdf. Accessed March 22, 2020Google Scholar
36 Triple Aim: The Best Care for the Whole Population at the Lowest Cost. Boston, Institute for Healthcare Improvement, 2020. http://www.ihi.org/Engage/Initiatives/TripleAim/Pages/default.aspx. Accessed March 22, 2020Google Scholar
37 : Reducing test utilization in hospital settings: a narrative review. Ann Lab Med 2018; 38:402–412Crossref, Medline, Google Scholar



