Identifying Young Adults at Risk of Medicaid Enrollment Lapses After Inpatient Mental Health Treatment
Abstract
Objective
This study sought to describe Medicaid disenrollment rates and risk factors among young adults after discharge from inpatient psychiatric treatment.
Methods
The sample included 1,176 Medicaid-enrolled young adults ages 18 to 26 discharged from inpatient psychiatric care in a mid-Atlantic state. Medicaid disenrollment in the 365 days postdischarge and disenrollment predictors from the 180-day predischarge period (antecedent period) were identified from administrative records. Classification and regression tree and probit regression analysis were used.
Results
Thirty-two percent were disenrolled from Medicaid within a year of discharge. Both analytical approaches converged on four main risk factors: being in the Medicaid enrollment category for persons with a nondisabled low-income parent or for a child in a low-income household, being age 18 or 20 at discharge, having a Medicaid enrollment gap in the antecedent period, and having no primary care utilization in the antecedent period. For the 48% of the sample continuously enrolled in the antecedent period who were in the enrollment categories for disabled adults or foster care children, the disenrollment rate was 13%.
Conclusions
A substantial minority of Medicaid-enrolled young adults discharged from inpatient care were disenrolled from Medicaid within a year. About half the sample had a low disenrollment risk, but the other half was at substantial risk. Risk factors largely reflected legal status changes that occur among these transition-age youths. Identifying inpatients at high risk of disenrollment and ensuring continuous coverage should improve access to needed postdischarge supports. Regular primary care visits may also help reduce unintended Medicaid disenrollment in this population.
Individuals maturing from adolescence to adulthood, referred to as young or emerging adults (1) or transition-age youths (2), undergo rapid legal and social status changes. Health care coverage is essential for young adults with chronic illnesses (1,3), especially those with serious mental health conditions, who often need a broad array of mental health, substance abuse, and medical treatments and rehabilitation services ( 4). However, in 2008 in the United States, 8.7 million persons ages 19 to 29 (19%) were uninsured and another 4.6 million (10%) were enrolled in Medicaid (5). Medicaid enrollment increases access to services and improves self-assessed somatic and mental health (6). Moreover, in contrast to many private insurers, Medicaid often covers the rehabilitative and supportive services that young adults with mental illness need, such as educational and employment supports (7). However, many low-income, young adults with serious mental health conditions are at risk of disruptions in Medicaid coverage.
Medicaid is offered principally to individuals made vulnerable by having low income or disability (5,8,9). Children predominate in Medicaid populations as a consequence of preferential eligibility under federal law (9). However, among Medicaid-covered individuals who are approaching legal adulthood, coverage is frequently withdrawn or reduced after a redetermination process at age 18 (9,10). Among Medicaid-enrolled 16-year-old mental health services users, disenrollment was shown to increase sharply at ages 18 and 19, with about half of females and two-thirds of males experiencing at least six months of disenrollment by age 19 (11). In addition, some states require age-based changes in enrollment categories at age 21 (for example, foster care coverage [12]). Moreover, gaps in insurance coverage (public or private) significantly diminish access to needed health care (13,14).
This study examined predictors of Medicaid disenrollment among young adults (ages 18 to 26) during the first year after discharge from inpatient mental health care. Information on disenrollment risk factors could be used to design enrollment supports for vulnerable young adults. The postdischarge year is a period of elevated suicide risk (15,16), and the risk is elevated further by discontinuity in outpatient care (17). Continuous Medicaid coverage may be an important prerequisite for timely postdischarge follow-up care, which research suggests reduces readmission risk (18). We hypothesized that the likelihood of disenrollment would be greater at ages associated with Medicaid eligibility changes (11), among males (11,19), among individuals not enrolled through a Medicaid disability category (11,19), among those with less serious psychiatric morbidity (11), and among those without recent connection to primary care or outpatient mental health services. We also expected that use of primary care and outpatient mental health clinic services would be correlated with continued enrollment in Medicaid because such safety-net providers—for example, federally qualified health centers—are adept at and often required by law to help clients enroll in Medicaid when they are eligible (20,21). Finally, we hypothesized that “near poor” individuals (22) (that is, individuals with incomes just above the poverty line) would be at increased disenrollment risk because even small income increases would render them ineligible for Medicaid (23).
Methods
Sample and variables
Administrative data from the Maryland Medicaid program and public mental health system were used to construct an individual-level database for all 1,177 Medicaid-enrolled persons who were ages 18 to 26 on discharge from an inpatient mental health stay between October 2005 and September 2006. For individuals with multiple admissions, only the first admission was used. One individual who was flagged as a qualified Medicare beneficiary (that is, limited Medicare and Medicaid coverage) was dropped, leaving 1,176 in the sample. The study was declared exempt from institutional review board review by the Maryland Department of Health and Mental Hygiene and the University of Maryland School of Medicine.
The dependent variable for this investigation was the occurrence of any days during which the person was not enrolled in Medicaid during the 365 days after discharge from the index inpatient admission. A one-year follow-up period was chosen because this interval represents heightened risk for suicide and hospital readmission (15,16,18,24).
Independent variables are listed in Table 1 and included demographic characteristics (age, race-ethnicity, gender, and urban-suburban versus rural residence), Medicaid eligibility category (25), and higher versus lower income. Several additional independent variables were obtained from antecedent records (the antecedent period was defined as the 180 days before the inpatient discharge) and included psychiatric morbidity (psychiatric diagnosis, co-occurring substance use diagnosis, and number of inpatient days), primary care and outpatient mental health care utilization, other medical service utilization (defined as in previous studies [26,27]), pregnancy, and Medicaid disenrollment.
| Independent variable | Description |
|---|---|
| Demographic characteristic | |
| Age | Age at discharge |
| Race | Reported in administrative record |
| Gender | Reported in administrative record |
| Urban-suburban versus rural residence | Based on zip code of residence at discharge |
| Higher incomeb | Family income at baseline >116% of the federal poverty level (FPL) or families with savings. Measured as being in a Medicaid eligibility category that includes families with incomes from 116% to 185% of the FPL (for example, children under age 19 or pregnant women) or in a “spend down” category in which families are required to use savings before becoming eligible for Medicaid |
| Medicaid eligibility category at discharge | |
| Disabled | Based on state or federal standards. Individuals in this category have higher overall morbidity than those in other eligibility categories. |
| Foster care | Custodial care provided by the state |
| Families and children or State Children’s Health Insurance Program | Based on family income and participant’s minor status |
| Limited coverage | Coverage is limited in duration or extent: pregnancy or postpartum, pharmacy assistance or primary care only, or noncitizens |
| Measured in antecedent periodc | |
| Psychiatric diagnosis | Based on the 5 most frequent diagnoses (ICD-9 codes) in the individual’s Medicaid claimsd |
| Schizophrenia spectrum disorder | ICD-9 codes 295.1–295.4 and 295.6–295.9 |
| Bipolar disorder | ICD-9 codes 296.0X, 296.4X–296.9X, absent a schizophrenia spectrum diagnosis |
| Depressive disorder | ICD-9 codes 296.2X–296.3X, 311.XX, absent a schizophrenia spectrum or bipolar disorder diagnosis |
| Other mental illness | ICD-9 codes 290, 293–4, 297–302, 306–319, absent a schizophrenia spectrum, bipolar, or depressive disorder diagnosis |
| Substance use disorder (not tobacco) | ICD-9 codes 303.XX–305.XX, excluding 305.1 (tobacco use disorder) |
| Pregnancyb | Based on HEDIS, ICD-9, or procedure codes in the individual’s record |
| Medicaid disenrollmentb | ≥1 days without Medicaid coverage per enrollment span records |
| Outpatient mental health service useb | Service for which the primary diagnosis was a psychiatric diagnosis (ICD-9 codes 290–302 and 306–319) and received in a standard outpatient mental health treatment venue (excluding emergency department, specialized day hospital, or psychiatric rehabilitation clinic) |
| Primary care visitb | Per definitions to isolate “well visits” and other primary care encounterse |
| Inpatient general medical stayb | Not connected to a primary psychiatric diagnosis (excluding ICD-9 codes 290–302, and 306–319) |
| Emergency department visitb | Per Uniform Bill revenue codes (045X or 0981)f |
| Total N of psychiatric inpatient days | Includes index hospitalization and all other inpatient days in the 180 days before the index hospitalization discharge for which the ICD-9 code for the primary diagnosis was 290–303 or 306–319 |
Statistical analysis
Three statistical approaches were used to characterize the relationship between postdischarge disenrollment and the independent variables. First, bivariate statistical tests (chi square or t tests) were used to compare all variables by disenrollment group (disenrolled versus not disenrolled). Second, classification and regression tree (CART) analysis, using SPSS, version 21, was conducted to display population subgroups and their relative risks of disenrollment. CART analysis creates statistically distinct subgroups based on sequential, hierarchical splits in the population that yield the strongest between-subgroup differences in regard to a selected outcome (28–30). This tree-growing method maximizes within-group homogeneity, and splits in the data were found based on squared probabilities of membership in each outcome category (using the Gini calculation) with a minimum change improvement of .0001. Only splits that produced final groups of at least 50 individuals were considered. The CART analysis provides a graphic that is useful for contrasting the relative risk of disenrollment between subgroups, but it does not yield point estimates that simultaneously adjust for all variables in the model.
The third approach was a probit regression analysis for the probability of disenrollment. Probit regression is similar to logistic regression but is based on the normal probability distribution and yields estimates that can be interpreted as changes in probability (rather than logistic regression odds ratios) (31). In addition to all the independent variables described above, this regression included an indicator for ages 18 or 20 at discharge, because eligibility for Medicaid under “child” coverage categories in Maryland often ends by ages 19 and 21 (25). For sensitivity analyses, probit regressions were reestimated with a disenrollment gap definition of ≥30 days. In addition, probit models were estimated without the limited-coverage group (composed largely of pregnant or postpartum women, which thus was correlated with the pregnancy status variable). Differences were considered significant if p values were ≤.05.
Results
Characteristics of the overall sample and disenrollment groups are presented in Table 2. The disenrollment rate in the 365-day postdischarge period was 32%.
| Variable | Total sample(N=1,176) | Bivariate analyses | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Continuously enrolled(N=797) | Disenrolled(N=379) | Probit multiple regressiona | |||||||||
| N | % | N | % | N | % | Test statistic | df | p | df/dxb | 95% CI | |
| Baseline | |||||||||||
| Male | 478 | 49 | 408 | 50 | 190 | 51 | χ2=.12 | 1 | .73 | .057 | –.008 to .120 |
| Age 18 or 20 | 300 | 26 | 169 | 21 | 131 | 35 | χ2=24 | 1 | <.001 | .130** | .045 to .220 |
| Age (M±SD) | 22.1±2.3 | 22.2±2.3 | 21.9±2.3 | t=2.1 | 1,174 | .04 | .015 | <–.001 to .030 | |||
| Race (reference: white) | χ2=5.8 | 4 | .21 | ||||||||
| White | 540 | 46 | 364 | 46 | 176 | 46 | |||||
| Black | 574 | 47 | 378 | 47 | 169 | 45 | .009 | –.055 to .073 | |||
| Hispanic | 31 | 2.6 | 16 | 2.0 | 15 | 3.9 | .150 | –.047 to .330 | |||
| Other | 18 | 1.5 | <11c | <2c | <11c | <3c | .220 | –.033 to .470 | |||
| Unknown | 40 | 3.4 | 29 | 3.6 | 11 | 2.9 | –.002 | –.170 to .160 | |||
| Higher income | 145 | 12 | 77 | 9.7 | 68 | 18 | χ2=16 | 1 | <.001 | .130* | .021 to .240 |
| Urban or suburban residence | 973 | 83 | 670 | 84 | 303 | 80 | χ2=3.0 | 1 | .081 | –.015 | –.092 to .063 |
| Diagnosis (reference: other mental illness)d | χ2=25 | 3 | <.001 | ||||||||
| Schizophrenia | 307 | 26 | 236 | 30 | 71 | 19 | –.006 | –.097 to .086 | |||
| Bipolar | 342 | 29 | 240 | 30 | 102 | 27 | .016 | –.065 to .097 | |||
| Depressive disorder | 238 | 20 | 150 | 19 | 88 | 23 | .027 | –.058 to .110 | |||
| Other mental illness | 289 | 25 | 171 | 21 | 118 | 31 | |||||
| Substance use disorder | 116 | 9.9 | 83 | 10 | 33 | 8.7 | χ2=.84 | 1 | .36 | –.036 | –.130 to .055 |
| Recent pregnancy | 135 | 11 | 107 | 13 | 28 | 7.4 | χ2=9.2 | 1 | .002 | –.150** | –.230 to –.058 |
| Enrollment category (reference: disabled)d | χ2=162 | 3 | <.001 | ||||||||
| Families and children or SCHIP | 382 | 32 | 165 | 21 | 217 | 57 | .380*** | .300 to .450 | |||
| Disabled | 646 | 55 | 514 | 64 | 132 | 35 | |||||
| Foster care | 58 | 4.9 | 53 | 6.7 | 5 | 1.3 | –.092 | –.240 to .057 | |||
| Limited coverage | 90 | 7.7 | 65 | 8.2 | 25 | 6.6 | .073 | –.077 to .220 | |||
| Antecedent period | |||||||||||
| Disenrollment | 354 | 30 | 176 | 22 | 178 | 47 | χ2=76 | 1 | <.001 | .170*** | .093 to .240 |
| Outpatient mental health visit | 977 | 83 | 699 | 88 | 278 | 73 | χ2=38 | 1 | <.001 | –.073 | –.160 to .011 |
| Primary care visit | 499 | 42 | 390 | 49 | 109 | 29 | χ2=43 | 1 | <.001 | –.110** | –.180 to –.047 |
| Inpatient general medical stay | 176 | 15 | 126 | 16 | 50 | 13 | χ2=1.4 | 1 | .24 | –.011 | –.095 to .073 |
| Emergency department visit | 486 | 41 | 340 | 43 | 146 | 39 | χ2=1.8 | 1 | .18 | .043 | –.022 to .110 |
| Inpatient psychiatric days (M±SD)e | 7.9±11 | 8.7±13 | 6.1±6.9 | t=3.7 | 1,174 | <.001 | –.004* | –.007 to –<.001 | |||
Unadjusted comparisons
Bivariate unadjusted comparisons indicated significant differences between individuals who were continuously enrolled and those who were disenrolled (Table 2). Disenrolled persons were more likely to be ages 18 or 20, to have a higher income, and to have had fewer inpatient psychiatric days. Those continuously enrolled were more likely to have a recent pregnancy and outpatient mental health or primary care visits in the antecedent period. Medicaid enrollment categories and mental health diagnoses were also differentially distributed among those continuously and discontinuously enrolled.
Regression tree results
Figure 1 summarizes the CART analysis results. The first and thus the most differentiating split was by enrollment category, indicating that the greatest difference in disenrollment rate was between the group that included individuals in the Medicaid category for families and children and individuals enrolled in the State Children’s Health Insurance Program (SCHIP) (F&C/SCHIP) (57% disenrolled) and the other enrollment categories (20% disenrolled). The absence of subsequent splits between the disabled, foster care, or limited-coverage Medicaid enrollment categories suggests that they were equivalent in regard to disenrollment risk. The CART analysis revealed a low-risk group (13% disenrollment): individuals who were not in the F&C/SCHIP category and who also did not have a disenrollment in the antecedent period. This low-disenrollment group was large (N=567, 48% of the sample) but contained only 18% of those who were disenrolled in the 365-day postdischarge period. By contrast, in the remaining sample (N=609), 51% were disenrolled. The highest disenrollment rate (83%) was observed for individuals in the F&C/SCHIP category who were between the ages of 20.1 and 22.7 and who had no primary care utilization in the antecedent period. This group accounted for only 7% of the sample. All other subgroups identified by the CART analysis experienced disenrollment at variously elevated rates (range 40%−71% disenrollment).
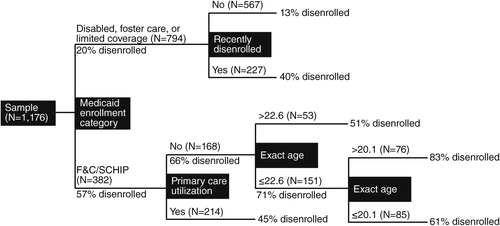
a F&C/SCHIP, in Medicaid category for families and children or in the State Children’s Health Insurance Program (SCHIP)
The CART analysis successfully classified 74% of the sample into the two categories (disenrolled or not), but successful classification of disenrollment occurred for only 38% of disenrolled cases.
Probit regression results
Table 2 also shows results of probit regression analyses of disenrollment. Marginal effects (df/dx) are reported for the probit analysis. Each marginal effect is the estimated change in the probability of disenrollment given a change in the value of a covariate, holding all other covariates constant at their sample mean values. For continuously valued covariates, df/dx corresponds to the change in disenrollment probability given that the covariate increases by 1 (for example, a one-year increase in age). For dichotomous covariates with values of 0 or 1, df/dx represents the difference in disenrollment probabilities for individuals with a value of 1 compared with individuals with a value of 0 (that is, the reference group). Results of both analyses were consistent with the CART results. The pseudo-R2 calculations indicated that the probit model accounted for 20% of the variance in the enrollment outcome (32). Of the ten variables that were significantly different between the enrolled and disenrolled groups in the bivariate analysis, seven were significantly different in the probit analysis; group differences in age (years), diagnoses, and outpatient mental health utilization did not reach significance in the probit analysis. Similar to the CART analysis, being in the F&C/SCHIP category predicted disenrollment: those in the F&C/SCHIP category were 37.6% more likely to be disenrolled than those not in this enrollment category (95% confidence interval [CI]=30.2%−44.9%). Also similar to the CART analysis, use of primary care in the antecedent period was associated with an 11.3% lower likelihood of postdischarge disenrollment (CI=17.9%−4.7%).
Probit sensitivity analyses
Sensitivity analyses (data not shown) largely agreed with results presented in Table 2. Removing the limited-coverage group (N=90) resulted in the following changes to disenrollment risk relative to the probit analysis results in Table 2: increased disenrollment risk was greater for higher income (increasing from 13% to 25%, CI=12%−38%) and for emergency department use in the antecedent period, which became significant (from 4% to 8%, CI=1%−15%) and lower for pregnancy, which became nonsignificant (from 15% to 9%, CI=–21% to 1%). Using a longer definition of disenrollment (≥30 days) replicated in magnitude and significance six of the seven significant effects listed in Table 2 (inpatient days became nonsignificant). Medicaid enrollment in the limited-coverage group, Hispanic race, and male gender were also significant correlates in the analysis that used a longer disenrollment period, suggesting that each variable had a stronger association with longer enrollment gaps than with shorter gaps. Longer disenrollment occurred for 28% of the sample.
Discussion
This study used two distinct statistical methods, which considered all independent variables hierarchically (CART analysis) or simultaneously (probit analysis), to quantify individual-level correlates of future Medicaid disenrollment among young adults who were discharged from a psychiatric inpatient stay. In the sample, 32% experienced disruptions in Medicaid coverage in the year after discharge. This finding alone supports concerns about the adequacy of health care coverage during this interval of heightened risk for suicide and hospital readmission (15,16,18,24).
Although the disenrollment rate in this sample is comparable to disenrollment rates observed in general populations of child and adult Medicaid enrollees (33), a relatively lower disenrollment rate was expected because of the multiple clinical vulnerabilities of these young adults. However, contrary to expectations, these young adults were not protected from disruptions in health care coverage. Moreover, young adults have been found to be less likely than any other age group to have private insurance (34), suggesting that in the critical time after inpatient mental health treatment, many individuals in the sample may have had poorer access to outpatient mental health treatment than other child or adult Medicaid enrollees.
Generally, our findings confirm five of the hypothesized risk factors. Support from both the CART and probit analyses confirmed that being “nondisabled” (that is, being enrolled in the F&C/SCHIP category), being at an age at which eligibility changes (18 or 20 years old), and not having a recent connection to primary care were each correlated with disenrollment. Probit analysis also indicated greater enrollment continuity among those with greater psychiatric morbidity (that is, more inpatient days) and less continuity with relatively high incomes. Less support was found for the effect of gender or for use of outpatient mental health services in the antecedent period.
Our findings indicate that the single strongest Medicaid disenrollment risk factor was being in the F&C/SCHIP category; most of the young adults (57%) in this category were subsequently disenrolled. To qualify for this enrollment category in this age group, most would either be a parent in a low-income family or a “child” in a low-income family. This state allows “children” in low-income families to remain covered by Medicaid up to age 21 if they remain a member of their parents’ (or other guardian’s) household. Thus some would lose eligibility by turning 18 when they have left the qualifying household, and others could remain covered until their 21st birthday if they remain in the household. The high risk for those at ages 18 and 20 suggests a strong contribution of these age-defined boundaries to disenrollment. Both analyses also converged on the importance of prior disenrollment as a risk factor for subsequent disenrollment. This finding suggests that being admitted for inpatient mental health treatment does not necessarily reduce future risk of disenrollment among young adults whose enrollment in Medicaid had been inconsistent. Having either of these two characteristics (being in the F&C/SCHIP or having an enrollment gap in the antecedent period) was associated with a 51% rate of disenrollment in the postdischarge period; approximately half the population had either of these two characteristics.
Primary care utilization in the antecedent period emerged as a factor protecting individuals from disenrollment. Primary care providers may observe the individual’s risk of coverage loss and may facilitate applications for continuation. Others have observed directly or commented about the importance of primary care, including holistic care, to help persons with serious mental illness address the other health issues they typically face (19,35–38).
The finding of lowered risk of disenrollment in the disabled and foster care groups and among individuals with more inpatient psychiatric days confirms that even within our clinically at-risk group, the most vulnerable individuals were less likely to be disenrolled. The surprisingly low disenrollment among foster care youths despite their “aging out” status, which was also reported by Pullmann and colleagues (11), may be accounted for by Medicaid extensions through age 20 for those who are disabled, pregnant, parents, or medically needy (39). For individuals in these particularly vulnerable subpopulations, case workers may undertake additional efforts to prevent disenrollment.
Pregnancy in the antecedent period also reduced disenrollment risk, consistent with previous findings in this age group (11) and for adults in general (20). Moreover, probit coefficients for pregnancy in the antecedent period were only slightly attenuated when the limited-coverage group was removed from the analysis. Pregnancy is a qualifying condition for limited coverage, and the limited-coverage group in this sample included 58 of the 135 pregnant women. Accordingly, it seems that any pregnancy, even if it was not the nominal Medicaid-qualifying event, resulted in more stable Medicaid enrollment. This finding suggests that new mothers or expectant women are easier to maintain in Medicaid than others, even though pregnancy-related eligibility often “expires” 60 days postpartum (25). Continued Medicaid enrollment may be supported through women’s own motivation to keep their infant and themselves covered or if they qualify as a low-income family when infant care can make earning income challenging.
The association of higher family income with greater disenrollment suggests “temporary” eligibility that results when slight fluctuations in income or age lead to disenrollment (23).
Overall, the findings of this study are similar to those found by Pullmann and colleagues (11), who examined Medicaid disenrollment patterns across 7.5 years for a Mississippi Medicaid cohort of 16-year-olds with mental health service utilization. These authors also found reduced disenrollment among individuals who were enrolled through disability or foster care or who were pregnant and substantial disenrollment at ages associated with enrollment eligibility changes and among those enrolled because of low family income. Generally, the direction of the effect of other variables measured in our study and in the study by Pullman and colleagues (male gender and schizophrenia diagnosis) was similar, but it was weaker in our study. Overall, the similarity of findings is striking given the shorter duration of disenrollment and follow-up in our study and the opposite state rankings of per capita income in the two samples (in the 2007 U.S. Census, Maryland ranked fifth and Mississippi 50th).
These findings suggest that Medicaid disenrollment after an inpatient stay might be prevented by identifying young adults who are at greatest risk of disenrollment and offering them enrollment supports. Such supports would involve assistance with Medicaid reenrollment or with obtaining alternative coverage and would presumably be offered by the state Medicaid office or the public mental health authority. Given the brevity of inpatient mental health treatment and the many competing priorities before discharge, assessing disenrollment risk should happen as quickly as possible, with linkage to supports that can advocate for health care coverage and help the individual negotiate for coverage.
Beginning in 2014, implementation of Medicaid expansions and insurance exchange plans under the 2010 Affordable Care Act might be expected to reduce the risk of Medicaid disenrollment among young adults. Many states are putting in place administrative processes intended to simplify health care plan enrollment (40,41). Examples of these processes include using a single unified application for both Medicaid and exchange plans and designing exchange plans specifically for youths under age 21. In addition, states can make childless adults with incomes up to 133% of the federal poverty level eligible for Medicaid, at state option, with a much higher federal match than for other populations and make persons who have been uninsured for more than six months potentially eligible for federally subsidized, high-risk, state insurance plans that provide coverage for individuals with preexisting conditions.
However, there are also reasons to be skeptical of the potential effectiveness of such reforms, at least for young adults with substantial psychiatric morbidity. Each step toward preventing disenrollment or obtaining alternative health care coverage requires individuals to engage in the application process, which may be a substantial barrier for this group. Indeed, studies of health care reform in Massachusetts have found increased enrollment for young adults in Medicaid and through health care exchanges (42,43) but worse enrollment among adults with behavioral health problems (44).
Several limitations should be noted. This sample comprised young adults in a single state’s Medicaid program, and the results may not generalize accurately to populations in other states, to other age groups, or to populations with different service utilization histories. In addition, the Medicaid enrollment data did not provide any information about receipt of care under private or other insurance coverage among those who disenrolled from Medicaid. However, evidence suggests that the likelihood of maintaining continuous health insurance coverage may have been quite low for these young adults, who were from low-income backgrounds and had serious mental health problems (34). Statistical models explained only a portion of the variability in Medicaid disenrollment, with most of the variability left unexplained. Factors such as disenrollment due to imprisonment (young adulthood is the peak age for imprisonment among males) and failure to reapply, which were not captured by this database, may also have been important.
Conclusions
This study provides evidence that gaps in Medicaid coverage among young adults in the year after an inpatient psychiatric discharge are related to being eligible for Medicaid because of low income, recent discontinuities in Medicaid enrollment, age associated with eligibility changes, and recent absence of primary care visits. In addition, having household income closer to the upper bound of Medicaid eligibility increased the risk of future Medicaid disenrollment, and pregnancy was only transiently protective against disenrollment.
Although implementation of the 2010 Affordable Care Act will offer various pathways for young adults to maintain their health care coverage, achieving this continuity may still be challenging for many because of their relative inexperience coupled with their psychiatric symptoms. In the absence of evidence demonstrating that the 2010 Affordable Care Act eliminates coverage disruptions in this vulnerable population, the feasibility and effectiveness of formal supports to increase continuity of coverage for needed mental health services should be examined.
1 : Emerging adulthood: a theory of development from the late teens through the twenties. American Psychologist 55:469–480, 2000Crossref, Medline, Google Scholar
2 : The transition to adulthood for youth who have serious emotional disturbance: developmental transition and young adult outcomes. Journal of Behavioral Health Services and Research 24:400–427, 1997Crossref, Google Scholar
3 : Global burden of disease in young people aged 10–24 years: a systematic analysis. Lancet 377:2093–2102, 2011Crossref, Medline, Google Scholar
4 Davis M, Green M, Hoffman C: The service system obstacle course for transition-age youth and young adults; in Transition of Youth and Young Adults With Emotional or Behavioral Difficulties: An Evidence-Based Handbook. Edited by Clark HB, Unruh D. Baltimore, Brookes, 2009Google Scholar
5 : Rite of Passage: Young adults and the Affordable Care Act of 2010. New York, Commonwealth Fund, 2010Google Scholar
6 : The Oregon health insurance experiment: evidence from the first year. Quarterly Journal of Economics 127:1057–1106, 2012Crossref, Medline, Google Scholar
7 : Health reform and the scope of benefits for mental health and substance use disorder services. Psychiatric Services 61:1081–1086, 2010Link, Google Scholar
8 : Better but Not Well: Mental Health Policy in the United States Since 1950. Baltimore, Johns Hopkins University Press, 2006Google Scholar
9 Aging out of Medicaid: What is the Risk of Becoming Uninsured? Pub no 8057. Menlo Park, Calif, Kaiser Commission on Medicaid and the Uninsured, 2010Google Scholar
10 : Health-related unmet needs of Supplemental Security Income youth after the age-18 redetermination. Health Services Research 46:1224–1242, 2011Crossref, Medline, Google Scholar
11 : Patterns of Medicaid disenrollment for youth with mental health problems. Medical Care Research and Review 67:657–675, 2010Crossref, Medline, Google Scholar
12 Courtney ME, Heuring DH: The transition to adulthood for youth “aging out” of the foster care system; in On Your Own Without a Net: The Transition to Adulthood for Vulnerable Populations. Edited by Osgood W, Foster EM, Flanagan C, et al. Chicago, University of Chicago Press, 2005Google Scholar
13 : US patterns of mental health service utilization for transition-age youth and young adults. Journal of Behavioral Health Services and Research 35:373–389, 2008Crossref, Medline, Google Scholar
14 : Children in the United States with discontinuous health insurance coverage. New England Journal of Medicine 353:382–391, 2005Crossref, Medline, Google Scholar
15 : Suicide after discharge from psychiatric inpatient care: a case-control study in Hong Kong. Australian and New Zealand Journal of Psychiatry 38:65–72, 2004Crossref, Medline, Google Scholar
16 : Mental health service delivery and suicide risk: the role of individual patient and facility factors. American Journal of Psychiatry 162:311–318, 2005Link, Google Scholar
17 : Review of predictors of suicide within 1 year of discharge from a psychiatric hospital. Current Psychiatry Reports 10:60–65, 2008Crossref, Medline, Google Scholar
18 : Post discharge follow-up of psychiatric inpatients and readmission in an HMO setting. Psychiatric Services 46:943–945, 1995Link, Google Scholar
19 : Cervical cancer screening and acute care visits among Medicaid enrollees with mental and substance use disorders. Psychiatric Services 63:815–822, 2012Link, Google Scholar
20 : Medicaid Outreach and Enrollment for Pregnant Women: What Is the State of the Art? Washington, DC, Urban Institute, 2009Google Scholar
21 : Potential Roles for Safety Net Providers in Supporting Continuity Across Medicaid and Health Insurance Exchanges. Portland, Me, National Academy for State Health Policy, 2012Google Scholar
22 : Insurance premiums and insurance coverage of near-poor children. Inquiry 43:362–377, 2006–2007Crossref, Medline, Google Scholar
23 Where Are States Today? Medicaid and CHIP Eligibility Levels for Children and Non-Disabled Adults. Menlo Park, Calif, Kaiser Commission on Medicaid and the Uninsured, 2012Google Scholar
24 : Predictors of receipt of aftercare and recidivism among persons with severe mental illness: a review. Psychiatric Services 47:487–496, 1996Link, Google Scholar
25 Quick Reference Guide to Medical Care Program Coverage Groups and Health Choice Eligibility. Baltimore, Maryland Department of Health and Mental Hygiene, 2006Google Scholar
26 HEDIS 2008: Technical Specifications (10284-100-08). Washington, DC, National Committee for Quality Assurance, 2007Google Scholar
27 : Primary care service areas: a new tool for the evaluation of primary care services. Health Services Research 38:287–309, 2003Crossref, Medline, Google Scholar
28 : Classification and Regression Trees. New York, Chapman and Hall/CRC, 1984Google Scholar
29 : Children at high risk for overweight: a classification and regression trees analysis approach. Obesity Research 13:1270–1274, 2005Crossref, Medline, Google Scholar
30 : A classification tree approach to the development of actuarial violence risk assessment tools. Law and Human Behavior 24:83–100, 2000Crossref, Medline, Google Scholar
31 : Limited-Dependent and Qualitative Variables in Econometrics. Cambridge, United Kingdom, Cambridge University Press, 1983Crossref, Google Scholar
32 Stata Annotate Output Probit Regression. Los Angeles, University of California, Los Angeles, Institute for Digital Research and Education, 2012Google Scholar
33 : Loss of health insurance among non-elderly adults in Medicaid. Journal of General Internal Medicine 24:1–7, 2009Crossref, Medline, Google Scholar
34 Mills RJ, Bhandari S: Health Insurance Coverage in the United States: 2002. Washington, DC, US Census Bureau, 2003Google Scholar
35 : Safety-net providers in some US communities have increasingly embraced coordinated care models. Health Affairs 31:1698–1707, 2012Crossref, Google Scholar
36 : About half of the states are implementing patient-centered medical homes for their Medicaid populations. Health Affairs 31:2432–2440, 2012Crossref, Medline, Google Scholar
37 : The role of psychiatric disorders in the relationship between cigarette smoking and DSM-IV nicotine dependence among young adults. Nicotine and Tobacco Research 10:439–446, 2008Crossref, Medline, Google Scholar
38 : Trajectories of change in obesity and symptoms of depression: the CARDIA study. American Journal of Public Health 100:1040–1046, 2010Crossref, Medline, Google Scholar
39 : Health insurance discontinuities among adolescents leaving foster care. Journal of Adolescent Health 44:41–47, 2009Crossref, Medline, Google Scholar
40 : Promise for the Future: How Federal Programs Can Improve the Career Outcomes for Youth and Young Adults With Serious Mental Health Conditions. Worcester, Mass, University of Massachusetts Medical School, and Washington, DC, Bazelon Center for Mental Health Law, 2013Google Scholar
41 Establishing Health Insurance Exchanges: An Overview of State Efforts. Menlo Park, Calif, Kaiser Family Foundation, 2013Google Scholar
42 : Have working-age people with disabilities shared in the gains of Massachusetts health reform? Inquiry 48:183–196, 2011Crossref, Medline, Google Scholar
43 : Disentangling the effects of health reform in Massachusetts: how important are the special provisions for young adults? American Economic Review 100:297–302, 2010Crossref, Medline, Google Scholar
44 : Sustaining enrollment in health insurance for vulnerable populations: lessons from Massachusetts. Psychiatric Services 64:360–365, 2013Link, Google Scholar



