Racial-Ethnic Differences in Treatment Initiation for New Diagnoses of Perinatal Depression
Abstract
Objective:
The adverse consequences of untreated perinatal depression highlight the need to identify populations to target in order to increase treatment rates. The authors sought to evaluate treatment initiation for a new diagnosis of depression during pregnancy or postpartum and to describe racial-ethnic differences in initiation and type (psychotherapy, antidepressants) of treatment in a large health care system with universal perinatal depression screening.
Methods:
This retrospective cohort study included women who delivered a live birth in the Kaiser Permanente Northern California system between October 2012 and May 2017. Black, Latina, Asian, and White women ages ≥15 years were eligible. New depression diagnoses were defined by using ICD-9 and ICD-10 codes from electronic health records. Treatment initiation was defined as receiving at least one antidepressant medication dispensation or psychotherapy visit up to 90 days after the diagnosis. Modified Poisson regression was used to estimate the risk for initiating treatment and the type of treatment initiated.
Results:
In total, 13,637 women with a new depression diagnosis (prenatal: N=7,041, 51.6%; postpartum: N=6,596, 48.4%) were identified. Of the pregnant women, 31.4% initiated treatment, and of the postpartum women, 73.1% initiated treatment. Latina and Asian women were less likely than White women to initiate treatment postpartum. During pregnancy and postpartum, non-White women were more likely to initiate psychotherapy. White women were more likely to initiate antidepressant medication during pregnancy and postpartum or a combination of antidepressant medication and psychotherapy during the postpartum period.
Conclusions:
Research is warranted to identify patient-, provider-, and system-level barriers that contribute to racial-ethnic disparities in perinatal mental health care.
HIGHLIGHTS
During the postpartum period, Latina and Asian women were less likely than White women to initiate treatment, and non-White women were more likely than White women to initiate psychotherapy.
Perinatal women’s preference for psychotherapy over antidepressant medication to manage new perinatal depression underscores the need for alternative evidence-based treatment options, such as mindfulness, exercise, and peer support.
The racial-ethnic differences in initiation of perinatal depression treatment highlight the need to identify patient-, provider-, and system-level barriers that contribute to these disparities.
Perinatal depression is a debilitating condition that affects 12%–20% of pregnant and postpartum women in the United States (1–4). The condition is associated with severe health consequences for both the mother and baby (5–8), highlighting the importance of treatment. However, less than half of women with prenatal depression and between 10% and 70% of women with postpartum depression initiate treatment. Furthermore, although racial-ethnic inequities in depression treatment are well documented in the general population (9, 10), two studies assessing these relationships among pregnant and postpartum women reported conflicting results (11, 12).
It is imperative to investigate the potential existence of racial-ethnic disparities in depression treatment during pregnancy and postpartum. Such investigations could inform interventions that increase treatment initiation and thereby improve the health of all women and their children. This study identified treatment initiation rates after a new depression diagnosis during pregnancy or postpartum overall and by depression severity. We describe racial-ethnic differences in treatment initiation and type of treatment (psychotherapy or antidepressant medication) within a health care system with universal perinatal depression screening. On the basis of the previous literature, we hypothesized that pregnant women of color would have lower rates of treatment initiation and be less likely to initiate antidepressant medication compared with pregnant White women.
Methods
Setting
This study was conducted within Kaiser Permanente Northern California (KPNC), a large integrated health care delivery system that provides medical care to >4.5 million members. All 15 regional service centers (and 48 associated office facilities) have obstetrics and gynecology departments as well as behavioral medicine and psychiatry departments. KPNC members are covered by employer-sponsored insurance plans, the insurance exchange, and Medicaid. Coverage is provided for approximately 40% of Northern California residents, and membership is similar to the population living in the geographic area (13). Information on diagnoses, outpatient visits, and prescribed medications is maintained within administrative and electronic health records (EHRs).
KPNC’s universal perinatal depression screening program screens women with the Patient Health Questionnaire–9 (PHQ-9), twice during pregnancy and 3–10 weeks postpartum (14, 15). The PHQ-9 is a validated instrument for depression screening across racial-ethnic groups (16) and has high sensitivity (>88%) and specificity (>88%) for obstetric patients (17, 18). For PHQ-9 scores ≥10, KPNC guidelines include symptom assessment and review of related medical history. A depression diagnosis is documented in the EHR on the basis of the screening score and clinical judgment. Treatment or referral are provided accordingly. Mental health care coverage includes individual and group psychotherapy, medication management, and prescriptions.
Study Design and Population
This population-based retrospective cohort study included women who delivered a live birth between October 7, 2012, and May 31, 2017. Black, Latina, Asian, and White women ages ≥15 years who were enrolled in the health plan for 6 months before their pregnancy and anytime within 90 days after the depression diagnosis were eligible (10). New depression diagnoses during the perinatal period were defined as those identified through ICD-9 and -10 codes anytime during pregnancy through 1 year postpartum (see the online supplement to this article), without evidence of a history of depression (diagnosis or treatment with antidepressant medication or psychotherapy) in the 6 months before pregnancy. Women with a new depression diagnosis between the first day of their last menstrual period and the day before delivery were included in the prenatal analyses. Those with a depression diagnosis after delivery through 1 year postpartum (and no depression diagnosis during pregnancy) were included in the postpartum analyses. Women belonging to racial-ethnic groups not listed above were excluded because of small samples. KPNC’s institutional review board approved the study and waived informed consent.
Measures
Race-ethnicity was based on self-report. Treatment initiation was defined as receiving at least one antidepressant medication dispensation or psychotherapy visit up to 90 days after the new depression diagnosis. Antidepressant medications included selective serotonin reuptake inhibitors, tricyclic acids, serotonin-norepinephrine reuptake inhibitors, monoamine oxidase inhibitors, and others (see the online supplement). A psychotherapy visit was defined as any visit >30 minutes with a CPT code (see the online supplement). Individual and group psychotherapies were covered by all insurance plans. Specifications for psychotherapy visits were based on research by the Mental Health Research Network (10).
Covariates
Covariates included the mother’s age at delivery; pre-pregnancy body mass index (underweight and normal weight, <25.0 kg/m2; overweight, 25.0–29.9 kg/m2; and obese, ≥30.0 kg/m2) (19); alcohol (yes or no), tobacco (yes or no), or other drug use (yes or no) during pregnancy; parity (number of previous pregnancies, 0, 1, ≥2); gestational age at prenatal care initiation; Medicaid status during pregnancy and postpartum; Charlson Comorbidity Index (CCI) score; and anxiety diagnoses during pregnancy and postpartum up to the date of the depression diagnosis. CCI scores were calculated on the basis of diagnosis codes identified in the EHR for the year before pregnancy, and the number of comorbid conditions was categorized as 0, 1, or ≥2 (20). The highest PHQ-9 score during pregnancy and postpartum recorded up to the date of the respective depression diagnosis was categorized as severe (≥15), moderate (10–14), or no-to-mild (<10) depressive symptoms (17). PHQ-9 scores were not available for all women.
Analysis
Chi-square and analysis of variance tests were conducted. Racial-ethnic differences in treatment initiation and type were assessed for the prenatal and postpartum periods separately. Point and interval estimates of relative risks for treatment initiation were obtained with modified Poisson regression with robust error variance (21), with and without adjustment for patient characteristics. Modified Poisson regression was used to estimate the likelihood for initiating each type of treatment, after adjustment for patient characteristics. Sensitivity analyses to address potential confounding by depression severity were conducted to adjust for PHQ-9 scores among women who had been screened with the PHQ-9 before their depression diagnosis. To assess whether the relationship between depression severity and treatment initiation differed by race-ethnicity, we conducted a likelihood ratio test comparing the full model (including the interaction term between severity and race-ethnicity) with the nested model (without the interaction term). Analyses were conducted in R, version 3.5.3.
Results
Among 126,032 eligible women, 13,637 (10.8%) had a new diagnosis of perinatal depression (Figure 1). Of this subset, 7,041 (51.6%) women had a new diagnosis during pregnancy (White, 42.9%; Latina, 30.7%; Asian, 13.8%; and Black, 12.6%), and 6,596 (48.4%) had a new diagnosis during the postpartum period (White, 38.2%; Latina, 32.8%; Asian, 18.7%; and Black, 10.2%). Descriptive characteristics of the sample are reported in Table 1. During pregnancy, Black women were more likely than Latina, White, and Asian women to have a missing PHQ-9 score (59% vs. 53%, 52%, and 48%, respectively, p<0.001), but no racial-ethnic differences were found during the postpartum period (54% vs. 55%, 51%, and 53%).
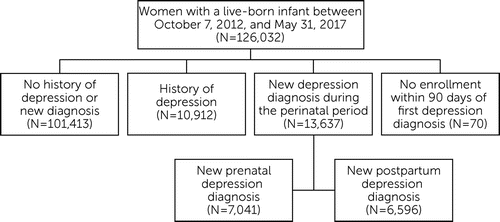
FIGURE 1. Study cohort flow diagrama
a Source: Authors’ analysis of data from the Kaiser Permanente Northern California electronic health record system.
| Total | White | Latina | Black | Asian | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Characteristic | N | % | N | % | N | % | N | % | N | % |
| Prenatal depression | ||||||||||
| Total | 7,041 | 100.0 | 3,018 | 42.9 | 2,164 | 30.7 | 884 | 12.6 | 975 | 13.8 |
| Maternal age at delivery (M±SD years) | 29.3±6.1 | 30.1±5.7 | 27.9±6.3 | 27.1±6.5 | 31.7±5.1 | |||||
| Pre-pregnancy BMI | ||||||||||
| Underweight or normal weight | 2,929 | 41.6 | 1,371 | 45 | 711 | 33 | 270 | 31 | 577 | 59 |
| Overweight | 1,909 | 27.1 | 789 | 26 | 638 | 30 | 237 | 27 | 245 | 25 |
| Obese | 2,060 | 29.3 | 804 | 27 | 764 | 35 | 358 | 41 | 134 | 14 |
| Missing | 143 | 2.0 | 54 | 2 | 51 | 2 | 19 | 2 | 19 | 2 |
| Substance use during pregnancy | ||||||||||
| Alcohol use | 791 | 11.2 | 353 | 12 | 238 | 11 | 107 | 12 | 93 | 10 |
| Tobacco use | 437 | 6.2 | 242 | 8 | 83 | 4 | 73 | 8 | 39 | 4 |
| Other drug use | 247 | 3.5 | 97 | 3 | 64 | 3 | 79 | 9 | 7 | 1 |
| Parityb | ||||||||||
| 0 | 3,065 | 43.6 | 1,454 | 48 | 839 | 39 | 334 | 38 | 438 | 45 |
| 1 | 2,149 | 30.5 | 947 | 31 | 633 | 29 | 261 | 29 | 308 | 32 |
| ≥2 | 1,557 | 22.1 | 500 | 17 | 626 | 29 | 249 | 28 | 182 | 19 |
| Missing | 270 | 3.8 | 117 | 4 | 66 | 3 | 40 | 5 | 47 | 5 |
| Medicaid coverage | 794 | 11.3 | 173 | 6 | 237 | 11 | 301 | 34 | 83 | 9 |
| Gestational age at prenatal care initiation (M±SD days) | 52.7±24.1 | 51.8±23.1 | 53.7±25.6 | 54.9±28.1 | 51.2±18.7 | |||||
| CCIc | ||||||||||
| 0 | 5,397 | 76.7 | 2,342 | 78 | 1,656 | 77 | 599 | 68 | 800 | 82 |
| 1 | 1,482 | 21.0 | 614 | 20 | 462 | 21 | 254 | 29 | 152 | 16 |
| ≥2 | 162 | 2.3 | 62 | 2 | 46 | 2 | 31 | 4 | 23 | 2 |
| Anxiety diagnosis | 206 | 2.9 | 113 | 4 | 55 | 3 | 14 | 2 | 24 | 3 |
| Depression symptom severityd | ||||||||||
| Severe | 368 | 5.2 | 118 | 4 | 136 | 6 | 49 | 6 | 65 | 7 |
| Moderate | 495 | 7.0 | 173 | 6 | 164 | 8 | 70 | 8 | 88 | 9 |
| None or mild | 2,485 | 35.3 | 1,164 | 39 | 723 | 33 | 244 | 28 | 354 | 36 |
| Missing | 3,693 | 52.4 | 1,563 | 52 | 1,141 | 53 | 521 | 59 | 468 | 48 |
| Postpartum depression | ||||||||||
| Total | 6,596 | 100.0 | 2,519 | 38.2 | 2,165 | 32.8 | 676 | 10.2 | 1,236 | 18.7 |
| Maternal age at delivery (M±SD years) | 30.3±5.5 | 30.6±5.1 | 29.3±5.9 | 29.2±6.3 | 32.0±4.5 | |||||
| Pre-pregnancy BMI | ||||||||||
| Underweight or normal weight | 2,669 | 40.5 | 1,134 | 45 | 649 | 30 | 172 | 25 | 714 | 58 |
| Overweight | 1,885 | 28.6 | 672 | 27 | 696 | 32 | 195 | 29 | 322 | 26 |
| Obese | 1,937 | 29.4 | 688 | 27 | 774 | 36 | 294 | 44 | 181 | 15 |
| Missing | 105 | 1.6 | 25 | 1 | 46 | 2 | 15 | 2 | 19 | 2 |
| Substance use during pregnancy | ||||||||||
| Alcohol use | 687 | 10.4 | 282 | 11 | 219 | 10 | 56 | 8 | 130 | 11 |
| Tobacco use | 196 | 3.0 | 109 | 4 | 39 | 2 | 26 | 4 | 22 | 2 |
| Other drug use | 91 | 1.4 | 37 | 2 | 23 | 1 | 25 | 4 | 6 | 1 |
| Parityb | ||||||||||
| 0 | 2,694 | 40.8 | 1,147 | 46 | 731 | 34 | 251 | 37 | 565 | 46 |
| 1 | 2,327 | 35.3 | 937 | 37 | 723 | 33 | 212 | 31 | 455 | 37 |
| ≥2 | 1,361 | 20.6 | 360 | 14 | 632 | 29 | 188 | 28 | 181 | 15 |
| Missing | 214 | 3.2 | 75 | 3 | 79 | 4 | 25 | 4 | 35 | 3 |
| Medicaid status | 1,258 | 19.1 | 365 | 14 | 423 | 20 | 386 | 57 | 84 | 7 |
| Gestational age at prenatal care initiation (M±SD days) | 51.6±22.7 | 49.8±19.0 | 53.0±25.7 | 53.5±25.5 | 52.2±22.1 | |||||
| CCIc | ||||||||||
| 0 | 5,411 | 82.0 | 2,087 | 83 | 1,761 | 81 | 519 | 77 | 1,044 | 85 |
| 1 | 1,076 | 16.3 | 402 | 16 | 364 | 17 | 142 | 21 | 168 | 14 |
| ≥2 | 109 | 1.7 | 30 | 1 | 40 | 2 | 15 | 2 | 24 | 2 |
| Anxiety diagnosis | 575 | 8.7 | 250 | 10 | 208 | 10 | 48 | 7 | 69 | 6 |
| Depression symptom severityd | ||||||||||
| Severe | 607 | 9.2 | 182 | 7 | 220 | 10 | 83 | 12 | 122 | 10 |
| Moderate | 570 | 8.6 | 195 | 8 | 199 | 9 | 70 | 10 | 106 | 9 |
| None or mild | 1,922 | 29.1 | 852 | 34 | 566 | 26 | 156 | 23 | 348 | 28 |
| Missing | 3,497 | 53.0 | 1,290 | 51 | 1,180 | 55 | 367 | 54 | 660 | 53 |
TABLE 1. Demographic characteristics of women with a new diagnosis of prenatal or postpartum depression, overall and by race-ethnicity, October 7, 2012, to May 31, 2017a
Treatment Initiation
Prenatal period.
Of the 7,041 women with a new prenatal depression diagnosis, 2,211 (31.4%) initiated treatment within 90 days of the diagnosis (Table 2). After we adjusted for covariates, we observed no differences in treatment initiation for Black or Asian women compared with White women (Black: adjusted relative risk [ARR]=1.07, 95% confidence interval [CI]=0.95–1.21; Asian: ARR=0.95, 95% CI=0.85–1.07). Compared with White women, Latina women were more likely to initiate treatment (ARR=1.10, 95% CI=1.01–1.20). After adjustment for depression severity, we observed no significant differences in treatment initiation for Latina, Black, or Asian women compared with White women (Table 2). Depression severity was statistically significantly associated with treatment initiation regardless of race-ethnicity (reference: PHQ-9 score <10; PHQ-9 score 10–14: ARR=1.54, 95% CI=1.35–1.73; PHQ-9 score ≥15: ARR=1.84, 95% CI=1.63–2.07; likelihood ratio test, p=0.997).
| Initiated treatment | ||||||||
|---|---|---|---|---|---|---|---|---|
| Race-ethnicity | N | % | Crude RR | 95% CI | ARRb | 95% CI | Sensitivity analysis ARRc | 95% CI |
| Prenatal depression (N=7,041) | ||||||||
| Overall | 2,211 | 31.4 | ||||||
| White (N=3,018; reference) | 921 | 30.5 | ||||||
| Latina (N=2,164) | 734 | 33.9 | 1.11 | 1.03–1.20 | 1.10 | 1.01–1.20 | 1.05 | .93–1.19 |
| Black (N=884) | 270 | 30.5 | 1.00 | .89–1.12 | 1.07 | .95–1.21 | 1.09 | .92–1.30 |
| Asian (N=975) | 286 | 29.3 | .96 | .86–1.07 | .95 | .85–1.07 | .98 | .84–1.14 |
| Postpartum depression (N=6,596) | ||||||||
| Overall | 4,820 | 73.1 | ||||||
| White (N=2,519; reference) | 1,919 | 76.2 | ||||||
| Latina (N=2,165) | 1,547 | 71.5 | .94 | .91–.97 | .93 | .90–.97 | .93 | .89–.98 |
| Black (N=676) | 502 | 74.3 | .97 | .93–1.02 | .98 | .93–1.03 | .99 | .93–1.05 |
| Asian (N=1,236) | 852 | 68.9 | .90 | .87–.94 | .91 | .87–.95 | .93 | .88–.98 |
TABLE 2. Association between race-ethnicity and treatment initiation within 90 days of a new prenatal or postpartum depression diagnosisa
Postpartum period.
Of the 6,596 women with a new postpartum depression diagnosis, 73.1% (N=4,820) initiated treatment within 90 days (Table 2). Latina and Asian women were less likely than White women to initiate treatment (Latina: ARR=0.93, 95% CI=0.90–0.97; Asian: ARR=0.91, 95% CI=0.87–0.95), whereas Black women were as likely as White women to initiate treatment (Black: ARR=0.98, 95% CI=0.93–1.03). Adjustment for depression severity yielded similar relationships (Latina: ARR=0.93, 95% CI=0.89–0.98; Asian: ARR=0.93, 95% CI=0.88–0.98; and Black: ARR=0.99, 95% CI=0.93–1.05). Women with higher depression severity were more likely to initiate treatment regardless of race-ethnicity (reference: PHQ-9 score <10; PHQ-9 score 10–14: ARR=1.03, 95% CI=0.98–1.08; PHQ-9 score ≥15: ARR=1.11, 95% CI=1.06–1.16; likelihood ratio test, p=0.938).
Treatment Type
Prenatal period.
Of the 2,211 women who initiated treatment during the prenatal period, 62% (N=1,360) started psychotherapy only, 21% (N=467) started antidepressant medication only, and 17% (N=384) started both (Figure 2). Significant racial-ethnic differences were found in the type of treatment initiated (see the online supplement). After we adjusted for covariates, women of color remained more likely to initiate psychotherapy only than White women (Latina: ARR=1.36, 95% CI=1.20–1.53; Black: ARR=1.50, 95% CI=1.27–1.77; and Asian: ARR=1.30, 95% CI=1.12–1.51). Adjustment for depression severity produced similar results.
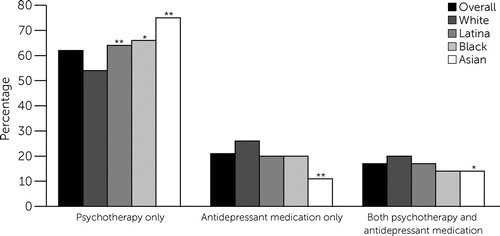
FIGURE 2. Prevalence of prenatal depression treatment type, overall and by race-ethnicitya
a Source: Authors’ analysis of data from the Kaiser Permanente Northern California electronic health record system. Asterisks indicate statistically significant percentage differences (reference: White women).
*p<0.05, **p<0.01.
After adjustment for covariates, women of color were less likely than White women to start antidepressant medication only (Latina: ARR=0.75, 95% CI=0.60–0.92; Black: ARR=0.59, 95% CI=0.43–0.80; and Asian: ARR=0.42, 95% CI=0.29–0.62). Similar relationships emerged when we adjusted for depression severity.
Compared with White women and after adjustment for covariates, Asian and Black women were less likely to initiate both psychotherapy and antidepressant medication; however, the findings for Black women did not reach statistical significance (Asian: ARR=0.66, 95% CI=0.47–0.94; Black: ARR=0.71, 95% CI=0.49–1.02). Similar results were obtained after adjustment for depression severity.
Postpartum period.
Of the 4,820 women who initiated treatment postpartum, 48% (N=2,295) started psychotherapy only, 19% (N=937) started antidepressant medication only, and 33% (N=1,588) initiated both (Figure 3). Significant racial-ethnic differences emerged for the type of treatment initiated (see the online supplement). After we adjusted for covariates, compared with White women, Latina, Black, and Asian women were significantly more likely to initiate psychotherapy (Latina: ARR=1.11, 95% CI=1.01–1.20; Black: ARR=1.30, 95% CI=1.16–1.46; and Asian: ARR=1.11, 95% CI=1.01–1.22). Similar findings emerged after adjustment for depression severity.
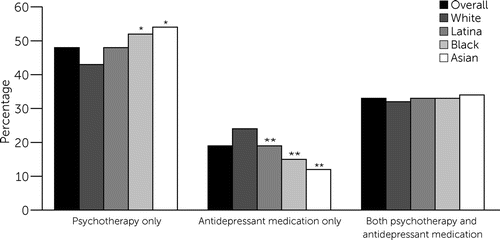
FIGURE 3. Prevalence of postpartum depression treatment type, overall and by race-ethnicitya
a Source: Authors’ analysis of data from the Kaiser Permanente Northern California electronic health record system. Asterisks indicate statistically significant percentage differences (reference: White women).
*p<0.05, **p<0.01.
Overall, Latina, Black, and Asian women were less likely to initiate antidepressant medication than were White women (Latina: ARR=0.62, 95% CI=0.54–0.71; Black: ARR=0.50, 95% CI=0.39–0.58; and Asian: ARR=0.47, 95% CI=0.38–0.58). These findings persisted after adjustment for depression severity.
No significant differences emerged in initiation of both psychotherapy and antidepressant medication between women of color and White women, after we adjusted for covariates. However, after adjustment for depression severity, Black women (ARR=0.78, 95% CI=0.61–0.99) were less likely than White women to initiate both antidepressant medication and psychotherapy; results for Latina women suggested a similar trend that did not reach statistical significance (ARR=0.89, 95% CI=0.77–1.04).
Discussion
In this study of women who delivered a live birth in the KPNC system, we documented low levels of treatment initiation for prenatal depression, and no significant racial-ethnic differences emerged. Despite overall high levels of initiation of postpartum depression treatment, Asian and Latina women were less likely than White women to begin treatment. Higher depression severity was associated with treatment initiation during pregnancy and postpartum, regardless of race-ethnicity. Moreover, Black, Asian, and Latina women were more likely than White women to initiate psychotherapy, whereas White women were more likely to initiate antidepressant medication without psychotherapy during pregnancy and with or without psychotherapy during the postpartum period.
Treatment Initiation
The observed rate of treatment initiation during pregnancy of 31.4% was equivalent to rates reported in a study conducted in hospital-based obstetrics clinics (22) but lower than the 50% reported in national samples (11, 23, 24). These differences may be due to variations in data collection or in the time frame for depression diagnosis and treatment. The national studies collected self-reported depression and treatment data for the previous 12 months (including before pregnancy), whereas this study used diagnoses and EHR data to identify treatment initiation within 90 days after depression diagnosis.
Conversely, we documented that nearly three-quarters of women with a new diagnosis of postpartum depression initiated treatment. This rate is higher than rates in previous reports that have documented that <10% of publicly insured women living in New Jersey initiated treatment within 6 months of delivery (12) and that 70% of privately insured and 50% of publicly insured women in a national sample initiated treatment within 90 days of a postpartum diagnosis (11).
Latina and Asian women were less likely than White women to initiate treatment for postpartum depression. Overall, we noted comparable rates of treatment initiation for Black and White women. Research on depression treatment in general populations (10) and perinatal populations (12) has found that Latina women are less likely than White women to initiate treatment. Our finding of similar rates of treatment initiation for Black and White women was comparable to findings in a study of pregnant women with private insurance or Medicaid (22) but contrasted with the results of a second study of a Medicaid-only sample, which reported that pregnant and postpartum Black women were less likely than White women to initiate treatment (12). The discrepancy with the second study may be due to differences in socioeconomic status, because our sample included women covered by either private insurance or Medicaid. To our knowledge, ours is the first study of depression treatment initiation during the perinatal period to include Asian women.
Treatment Type
Women of color were more likely than White women to initiate psychotherapy only, whereas White women initiated antidepressant medication treatment alone at higher rates compared with women from other racial-ethnic groups. These findings are consistent with those of previous studies of nonpregnant (10) and postpartum women (12).
Implications
The low rates of prenatal depression treatment initiation found in this study suggest the need to identify specific treatment barriers during pregnancy. The lower rates could have been partially due to concerns over the safety of antidepressant medication during pregnancy (25, 26), because rates of any antidepressant use were higher in the postpartum period. Low rates of prenatal depression treatment are concerning given that prenatal depression is the largest risk factor for postpartum depression (27).
The divergent patterns of the treatment type initiated may suggest that women of color request or are offered psychotherapy more often, or are more amenable to it, than White women. These patterns may also reflect that White women are more likely to be offered or more willing to fill an antidepressant medication prescription compared with women of color. A large majority of White women initiated psychotherapy alone or in combination with antidepressants, whereas ≤50% of Latina, Black, or Asian women initiated antidepressants during pregnancy or postpartum. Access to preferred treatment choice improves treatment initiation, adherence, and outcomes (28, 29). Women’s preference for nonpharmaceutical treatment options during the perinatal period (26) highlights the need for evidence-based research into alternative treatment options, such as mindfulness, exercise, or peer support.
Lack of health insurance contributes to racial-ethnic disparities in mental health care. Given that this study was conducted in an insured population, our findings suggest the need to identify other factors that contribute to the disparities we observed, especially among women in the perinatal period. Financial circumstances, inflexible work schedules, and lack of childcare have been identified as barriers to perinatal depression treatment (30), especially among women of color (26). Addressing these barriers and understanding how cultural beliefs, racial-ethnic differences in patient perceptions and experiences of mental health and motherhood, depression stigma, patient-provider communication, and institutional racism in the health care system contribute to these disparities are necessary to increase treatment rates and reduce disparities (26, 31).
Women of color often report negative interactions with the health care system during pregnancy, including experiences of racism, unmet information needs, and stressful interactions with staff, which may contribute to differential treatment decisions by race and ethnicity (32–34). Non-White patients have reported a general distrust in the ability of the majority-White medical establishment to appropriately meet their health care needs (26). Additionally, cultural differences may be a factor in decisions regarding treatment initiation. Qualitative research has documented that Latina patients report that they declined treatment because of family expectations that they were responsible for parenting duties, leaving no time for treatment (26).
Strengths and Limitations
Study limitations included the inability to capture brief treatment provided by the obstetrician-gynecologist or psychotherapy received outside of KPNC that was not paid for by Kaiser Permanente. We do not know whether more affluent women paid out of pocket to receive psychotherapy outside of KPNC. If so, the disparities in treatment initiation may be greater than reported here and may explain the few differences in treatment initiation during pregnancy and between Black and White women postpartum. This possible unobserved difference may also have decreased the differences noted between non-White and White women in initiation of postpartum psychotherapy. However, our study captured psychotherapy received outside of the health care system that was paid for by Kaiser Permanente. Additionally, Medicaid beneficiaries—a small portion of women at the beginning of the study period—received mental health care outside of KPNC, which was not captured in our study. We did not have information on non-evidence-based treatment received, such as mindfulness interventions or religious support, whose utilization may differ across racial-ethnic groups (26, 35). Additionally, prescriptions filled outside of the health plan were not captured. However, most KPNC members (>96%) fill their prescriptions within the health care system (36). We do not know the reasons for failure to initiate treatment, nor do we know the role of the patient, provider, or health care system in lack of treatment initiation overall or for the differences in treatment initiation by race-ethnicity.
The study period overlapped with the period for implementation of the perinatal depression screening program. Screening scores may not have been entered into the EHR while clinic workflows were being developed. Thus, PHQ-9 scores were not available for all women, and pregnant Black women were less likely to have a screening score. However, all women in this study had a new depression diagnosis, and depression was therefore addressed by the clinician during a perinatal care visit. Of note, our previous work documented that 97% of women were screened for perinatal depression at least once during pregnancy or postpartum (15), as recommended by the U.S. Preventive Services Task Force (37).
Our findings were strengthened by the use of EHR data to ascertain perinatal depression diagnoses, depression severity scores, and covariates such as Medicaid status and comorbid anxiety and by the focus on the prenatal and postpartum periods. KPNC’s integrated health care delivery system has been influential in the development and diffusion of new models of care and has provided a setting to study innovative approaches to health care delivery (38, 39). Research conducted in integrated health care systems has been disseminated to other settings; thus, these findings have important implications outside of KPNC.
Conclusions
This study identified low rates of treatment initiation for prenatal depression, racial-ethnic inequities in postpartum depression treatment initiation, and racial-ethnic inequities in perinatal treatment type in a large integrated health care delivery system with a program for universal perinatal depression screening designed to enhance identification and care. These findings signify the need for research to identify patient-, provider-, and system-level barriers that contribute to racial-ethnic disparities in perinatal mental health care; findings from such research could inform the development of programs and policies to improve the health of all women and their children.
1. : Perinatal depression: a systematic review of prevalence and incidence. Obstet Gynecol 2005; 106:1071–1083Crossref, Medline, Google Scholar
2. : Perinatal depression: prevalence, screening accuracy, and screening outcomes. Evid Rep Technol Assess 2005; 119:1–8Medline, Google Scholar
3. The American College of Obstetricians and Gynecologists Committee Opinion no 630. Screening for perinatal depression. Obstet Gynecol 2015; 125:1268–1271Crossref, Medline, Google Scholar
4. : Racial and ethnic differences in factors associated with early postpartum depressive symptoms. Obstet Gynecol 2005; 105:1442–1450Crossref, Medline, Google Scholar
5. : Onset timing, thoughts of self-harm, and diagnoses in postpartum women with screen-positive depression findings. JAMA Psychiatry 2013; 70:490–498Crossref, Medline, Google Scholar
6. : The impact of postnatal depression on infant development. J Child Psychol Psychiatry 1992; 33:543–561Crossref, Medline, Google Scholar
7. : The influence of maternal depression, caregiving, and socioeconomic status in the post-natal year on children's language development. Child Care Health Dev 2008; 34:603–612Crossref, Medline, Google Scholar
8. : The effect of postpartum depression on child cognitive development and behavior: a review and critical analysis of the literature. Arch Womens Ment Health 2003; 6:263–274Crossref, Medline, Google Scholar
9. : Racial and ethnic differences in utilization of mental health services among high-risk youths. Am J Psychiatry 2005; 162:1336–1343Link, Google Scholar
10. : Treatment initiation for new episodes of depression in primary care settings. J Gen Intern Med 2018; 33:1283–1291Crossref, Medline, Google Scholar
11. : Diagnosis of postpartum depression and timing and types of treatment received differ for women with private and Medicaid coverage. Womens Health Issues 2018; 28:524–529Crossref, Medline, Google Scholar
12. : Racial and ethnic disparities in postpartum depression care among low-income women. Psychiatr Serv 2011; 62:619–625Link, Google Scholar
13. : The Kaiser Permanente Northern California adult member health survey. Perm J 2016; 20:15–225Crossref, Medline, Google Scholar
14. : Perinatal obstetric office depression screening and treatment: implementation in a health care system. Obstet Gynecol 2016; 127:911–915Crossref, Medline, Google Scholar
15. : Improved perinatal depression screening, treatment, and outcomes with a universal obstetric program. Obstet Gynecol 2016; 127:917–925Crossref, Medline, Google Scholar
16. : Using the Patient Health Questionnaire–9 to measure depression among racially and ethnically diverse primary care patients. J Gen Intern Med 2006; 21:547–552Crossref, Medline, Google Scholar
17. : The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 2001; 16:606–613Crossref, Medline, Google Scholar
18. : Validity and utility of the PRIME-MD Patient Health Questionnaire in assessment of 3,000 obstetric-gynecologic patients: the PRIME-MD Patient Health Questionnaire Obstetrics-Gynecology Study. Am J Obstet Gynecol 2000; 183:759–769Crossref, Medline, Google Scholar
19. Defining Adult Overweight and Obesity. Atlanta, Centers for Disease Control and Prevention, 2017. https://www.cdc.gov/obesity/adult/defining.html. Accessed Aug 25, 2022 Google Scholar
20. : A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40:373–383Crossref, Medline, Google Scholar
21. : A modified Poisson regression approach to prospective studies with binary data. Am J Epidemiol 2004; 159:702–706Crossref, Medline, Google Scholar
22. : Rates and predictors of depression treatment among pregnant women in hospital-affiliated obstetrics practices. Gen Hosp Psychiatry 2006; 28:289–295Crossref, Medline, Google Scholar
23. : Depression and treatment among US pregnant and nonpregnant women of reproductive age, 2005–2009. J Womens Health 2012; 21:830–836Crossref, Medline, Google Scholar
24. : Mental health treatment and unmet mental health care need among pregnant women with major depressive episode in the United States. Psychiatr Serv 2019; 70:503–506Link, Google Scholar
25. : Preferences and attitudes toward approaches to depression relapse/recurrence prevention among pregnant women. Behav Res Ther 2014; 54:7–11Crossref, Medline, Google Scholar
26. : Engagement in perinatal depression treatment: a qualitative study of barriers across and within racial/ethnic groups. BMC Pregnancy Childbirth 2021; 21:512Crossref, Medline, Google Scholar
27. : Predictors of postpartum depression: an update. Nurs Res 2001; 50:275–285Crossref, Medline, Google Scholar
28. : Patients’ depression treatment preferences and initiation, adherence, and outcome: a randomized primary care study. Psychiatr Serv 2009; 60:337–343Link, Google Scholar
29. : The influence of patient preference on depression treatment in primary care. Ann Behav Med 2005; 30:164–173Crossref, Medline, Google Scholar
30. : Women’s attitudes, preferences, and perceived barriers to treatment for perinatal depression. Birth 2009; 36:60–69Crossref, Medline, Google Scholar
31. : Can quality improvement programs for depression in primary care address patient preferences for treatment? Med Care 2001; 39:934–944Crossref, Medline, Google Scholar
32. : Socially disadvantaged women’s views of barriers to feeling safe to engage in decision-making in maternity care. Women Birth 2014; 27:132–137Crossref, Medline, Google Scholar
33. : Information and power: women of color’s experiences interacting with health care providers in pregnancy and birth. Soc Sci Med 2019; 238:112491Crossref, Medline, Google Scholar
34. : Health care experiences of pregnant, birthing and postnatal women of color at risk for preterm birth. Soc Sci Med 2018; 201:127–135Crossref, Medline, Google Scholar
35. : Family culture in mental health help-seeking and utilization in a nationally representative sample of Latinos in the United States: the NLAAS. Am J Orthopsychiatry 2014; 84:353–363Crossref, Medline, Google Scholar
36. : New prescription medication gaps: a comprehensive measure of adherence to new prescriptions. Health Serv Res 2009; 44:1640–1661Crossref, Medline, Google Scholar
37. : Screening for depression in adults: US Preventive Services Task Force recommendation statement. JAMA 2016; 315:380–387Crossref, Medline, Google Scholar
38. : Effect of primary health care orientation on chronic care management. Ann Fam Med 2006; 4:117–123Crossref, Medline, Google Scholar
39. : Treatment intensification and risk factor control: toward more clinically relevant quality measures. Med Care 2009; 47:395–402Crossref, Medline, Google Scholar



