Barriers to Integrated Medication-Assisted Treatment for Rural Patients With Co-occurring Disorders: The Gap in Managing Addiction
Abstract
Objective:
Guidelines for treatment of opioid use disorder stipulate for mental health assessment and the option for treatment alongside medication for opioid use disorder (MOUD). Yet efforts to expand MOUD treatment capacity have focused on expanding the workforce of buprenorphine providers. This article aims to describe the processes facilitating and impeding integrated care for rural patients with co-occurring opioid use disorder and mental health conditions.
Methods:
Qualitative interviews were conducted with primary care and specialty providers (N=26) involved in integrated care through the state’s hub-and-spoke system and with system-level stakeholders (N=16) responsible for expanding access to MOUD in rural California.
Results:
Rural primary care providers struggled to offer adequate mental health resources to patients with co-occurring conditions because of personnel shortages and inadequate availability of telehealth. Efforts to intensify care through referral to county mental health systems and private community providers were thwarted by access barriers. The bifurcated nature of treatment systems resulted in inadequate training in integrated care and the deprioritization of mental health in patient evaluations.
Conclusions:
Significant system-level barriers undermine the implementation of integrated MOUD in rural areas, potentially increasing the suffering of residents with co-occurring conditions and intensifying burnout among providers.
HIGHLIGHTS
Few people with co-occurring mental illness and opioid use disorder receive integrated care for both conditions.
Significant system-level barriers undermine the implementation of integrated medication-assisted treatment for opioid use disorder in rural areas.
These gaps potentially increase the distress of people in rural areas with co-occurring conditions and intensify burnout among rural providers.
Nearly two-thirds of adults with opioid use disorder had past-year mental illness (1). Clinical guidelines for treating opioid use disorder emphasize the importance of offering psychosocial needs assessment and the option for mental health treatment alongside medication for opioid use disorder (2, 3). Integrated care treats substance use and mental health simultaneously, involving the same providers in treatment activities that address both conditions. No extant randomized controlled trials have compared integrated and nonintegrated mental health treatment alongside buprenorphine treatment, even though broader research demonstrates that integrated behavioral health treatment leads to improved outcomes for people with co-occurring substance use and mental health conditions (4–6). Still, a recent study found that only one-quarter of people with co-occurring mental illness and opioid use disorder received past-year treatment for both conditions (7). Integrated service delivery is the exception rather than the rule in U.S. health care settings (8, 9), with one study finding that only 23% of primary care providers surveyed met criteria for being able to treat people with co-occurring conditions (10).
Accordingly, efforts have focused on offering integrated, stepped behavioral health treatments in the primary care settings, where most people access health care. As shown in Figure 1, providers address mild to moderate co-occurring conditions as they emerge in primary care settings and refer patients with severe needs to external behavioral health specialists, intensifying care in steps, depending on patient need (11). The most effective stepped care models for mental health involve a care manager who coordinates between primary care providers and specialists, promotes self-management among patients, and documents the evolution of patient conditions (12). Stepped, coordinated care approaches also have been effective for opioid use disorder (13), particularly when dedicated care managers coordinate patient care (14, 15). Yet most research on expanding access to medication for opioid use disorder (MOUD) has focused on increasing the number of MOUD providers in primary care settings, because a waiver (“x-waiver”) from the U.S. Drug Enforcement Administration is required to prescribe buprenorphine (16–24). Little is known about the implementation strategies necessary to support stepped, coordinated approaches that facilitate integrated care of opioid use disorder and co-occurring mental illness in primary care settings, despite their prevalence. Even fewer studies have examined how organizations in low-resource settings, such as rural areas, attempt to integrate care for patients with co-occurring opioid use disorder and mental disorders.
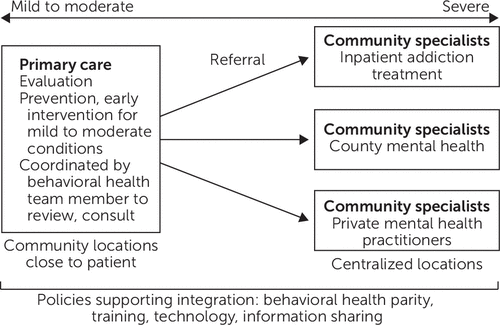
FIGURE 1. Model of stepped behavioral health integration in primary carea
aSource: McGovern et al. (11). Recent policy changes have enabled the potential to offer integrated care for co-occurring mental and opioid use disorders in the primary care settings most accessible to patients. Primary care facilitates screening and care for patients with mild to moderate conditions. For more advanced care, steps to intensify care are made through referral to community specialists.
This gap is critical for rural populations with opioid use disorder, which face a higher prevalence of mental disorders, including suicide (25, 26), serious psychological distress (27), and co-occurring conditions (28, 29). Most efforts to expand MOUD in rural communities have focused on access to medication (17, 22–24) rather than on MOUD integrated with mental health care. The deep disparities inherent in rural health service infrastructures (30, 31) severely restrict integrated MOUD in rural areas. With widespread shortages of mental health clinicians (32), patients in rural areas receive less mental health treatment (33) and may cease seeking care because of negative treatment experiences (34).
Recent systemic efforts to expand primary care–based MOUD in nonurban communities, such as in hub-and-spoke systems, have been lauded for building pathways to integrated care within a continuum of care based on need (35, 36). Such systems assign patients with acute, complex needs to “hubs” with addiction and psychiatric expertise and assign stabilized patients to primary care–based “spokes” that offer buprenorphine and community supports, adjusting patients’ locations as their needs change. This continuum of care is intended to mobilize resources to match patient needs while creating interorganizational relationships that enable integrated care. As investments in rural MOUD expand, particularly through hub-and-spoke networks, we sought to understand the processes facilitating and impeding integrated care for rural patients with co-occurring opioid use disorder and mental health conditions. Specifically, we asked, How do rural primary care organizations facilitate integrated, stepped care for patients with co-occurring conditions? and What systemic factors influence the provision of such care? This study can guide future research to systematically explore barriers and facilitators to integrated MOUD in underresourced rural areas.
Methods
Qualitative implementation research is suited to exploring the barriers and facilitators to the uptake and sustainment of evidence-based practices (37) through a detailed description of the organizational and systemic contexts that shape their use (38). We conducted semistructured interviews in 2018–2019 with health care providers (N=26) and system-level stakeholders (N=16) involved in expanding access to MOUD in rural California through the state’s hub-and-spoke system. The larger study from which we drew our data was informed by the exploration, preparation, implementation, and sustainment (EPIS) conceptual framework (39, 40) in order to isolate the organizational- and system-level constructs relevant to the integration of MOUD and to identify facilitators and barriers to integration. This framework captures the long-term process in which stakeholders explore intervention options, prepare for implementation, implement the intervention, and sustain the intervention. This study took place during implementation, but participants reflected on the exploration and preparation phases and anticipated future sustainment on the basis of current experiences. A majority of participants worked in census tracts defined as rural in accordance with the U.S. Office of Management and Budget’s rural-urban commuting area codes 4–7. After we applied implementation science sampling techniques to highlight a range of perspectives relevant to implementation (37), our purposive sampling was oriented toward recruiting providers with diverse roles (Table 1) along the continuum of primary care–based integrated care (Figure 1) and system-level stakeholders with community and administrative expertise (e.g., administrators, public health officials, harm reduction advocates) related to integrated treatment for MOUD. As described elsewhere (41), participants were recruited from regions served by four of the five hub-and-spoke systems in California serving rural areas and provided informed consent. This study was approved by the institutional review board at the University of California, Berkeley.
| Characteristic | N | % |
|---|---|---|
| Provider | 26 | 62 |
| System-level stakeholder | 16 | 38 |
| Gender | ||
| Female | 36 | 86 |
| Male | 6 | 14 |
| Race-ethnicity | ||
| White, non-Hispanic | 22 | 52 |
| White, Hispanic | 11 | 26 |
| African American | 3 | 7 |
| American Indian | 1 | 2 |
| Other | 2 | 5 |
| Missing | 3 | 7 |
| Provider type | ||
| Physician | 9 | 35 |
| Mental health specialist/case manager | 6 | 23 |
| Nurse | 5 | 19 |
| Physician’s assistant | 1 | 4 |
| Substance use counselor | 2 | 8 |
| Frontline staff | 3 | 11 |
| System-level type | ||
| Providing organization administrator | 8 | 50 |
| Public health | 4 | 25 |
| Harm reduction | 4 | 25 |
| Organization (all participants)a | ||
| FQHCb | 18 | |
| Public health (county, state) | 4 | |
| Behavioral health (county mental health) | 2 | |
| Private practice (primary care, mental health) | 6 | |
| For profit (e.g., start-up, for-profit methadone) | 4 | |
| Recovery organization | 3 | |
| Consumer/advocacy organization | 6 |
TABLE 1. Characteristics of integrated care providers and system-level stakeholders in rural California (N=42)
Participants were recruited by phone and e-mail. Interviews, informed by constructs from the EPIS framework, explored the background of patients served, the implementation of MOUD, implementation strategies for integrating care (e.g., supporting referral through warm handoffs, creating relationships with regional providers), and treatment philosophy. Interviews were recorded, transcribed, and entered into Dedoose qualitative data analysis software. After reading transcripts, we created a codebook of sensitizing concepts (42) from the implementation science literature (40) and of aspects of integrated care (11, 12), such as components of MOUD implementation funding sources, and methods for coordinating care. A team of coders defined and refined the codes and then applied codes to the data by using memos to document analytical choices. Coders reviewed and discussed a subset of the other’s code applications. Then we identified subcodes to deepen our understanding of themes from the interviews.
Results
Our results, summarized in Figure 2, are organized around three thematic areas: primary care–based resources, gaps in the continuum of care, and the bifurcation of the health system.
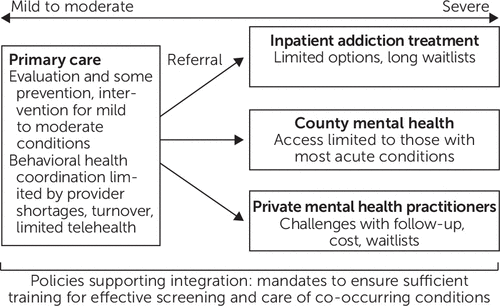
FIGURE 2. Summary of results of intervention providing integrated care to rural patients with co-occurring opioid use disorder and mental health conditionsa
aSource: McGovern et al. (11). Across the continuum of care, multiple shortages and policy gaps limit the capacity to provide integrated behavioral health care in primary care settings most accessible to rural patients with co-occurring mental illness and opioid use disorder.
Primary Care–Based Resources
Primary care provider shortages.
Administrators in organizations serving rural populations often have had to deal with recruiting and retaining x-waivered providers and primary care providers with mental health training (e.g., nurses, social workers, psychiatrists) when both were in short supply. Although many rural practices have included an x-waivered provider, practices in more remote areas have remained in a precarious circumstance, always one step away from their only waivered provider retiring, moving, or passing away. The backgrounds of primary care providers with mental health expertise ranged from training in psychiatry or a psychology specialty to, more commonly, training in master’s-level social work, case management, or another form of counseling. Because MOUD programs require multiple personnel, some organizations faced extensive provider shortages that limited their capacity. “I don’t think we’ve ever been fully staffed,” commented one nurse coordinator, noting the long period that the MOUD program of the coordinator’s federally qualified health clinic had lacked personnel for six positions, including drug counselors, therapists, and nurses.
Challenges to integrating primary care.
Participants described how organizational models of care were built around screening, some in-house therapy and psychiatric medicine management, and referral, with extremely limited resources for escalating care. One physician reflected cynically on the recent expansion of resources for MOUD and concluded, “The upshot is, psych is the one big gap in dealing with addiction.” Most programs required all patients with opioid use disorder to take part in behavioral health services, such as individual or group sessions, with a drug counselor or in mental health services with a social worker or psychiatrist, regardless of whether the patient had a co-occurring mental disorder. Yet behavioral health, broadly defined, was offered as a “soft” requirement at some organizations. One primary care provider described the process with patients stating, “They have the option. ‘Are you interested in behavioral health services? Is it something you’d like to do? We can schedule an appointment right now.’ ”
Providers cited challenges that kept them from offering more in-house mental health resources, including workforce shortages, inadequate time to deliver more case management, and sharing mental health providers with other organizations. Although provider participants were involved in the state’s hub-and-spoke system, the system offered no funding or staffing explicitly for mental health care. Organizations with mental health resources judiciously scheduled personnel with expertise in co-occurring conditions. “We have other therapists,” one participant described, “but because [of] the complexity of these patients [who receive MOUD], [one therapist is] the one that sees them.” The participant clarified that “there’s a lot of double- and triple-booking” on the 1.5 days a week this therapist was present in the clinic. For patients with established relationships with the primary care providers they were already seeing, receiving a referral reportedly provoked fear and discomfort. One clinic manager discussed the challenge of balancing patients’ needs for specialty services (e.g., trauma-informed care) with their preferences, noting that patients ask, “Can’t we just increase counseling here?” Recognizing the need for more extensive in-house behavioral health support, providers felt powerless. Referring patients elsewhere represented a risky prospect, because multiple barriers would prevent most patients from getting care.
Expanding resources through hiring and telemedicine.
Several participants described how their organization’s ability to hire a psychiatrist transformed care. Telemedicine was often described by participants as an option that their organizations were exploring rather than implementing. Many participants described how telemedicine options varied over time within organizations because of turnover or changes in the equipment. Others described how inadequate relationship building between community-based providers and remotely located telemedicine providers could have adverse impacts on patients. “Frequently, the medications get messed up,” explained one physician, because “the psychiatrist is not that familiar with the patient, and there’s not enough chance to review the chart and discuss with family or local counselors.”
Gaps in the Continuum of Care
At the time of our study, California was engaged in multiple initiatives to build a continuum of care for behavioral health, including a Medicaid waiver that restructured payment and development of a hub-and-spoke network. Participants commented that such efforts vastly underestimated the lack of resources in rural areas. Referring to the state’s hub-and-spoke network, one administrator-provider noted, “What a hub-and-spoke model really speaks about is levels of care stepped down or [stepped] up levels of care, and right now we’re an island. We do what we can do, and we do the best we can because there isn’t much else anywhere.” Many providers were frustrated with unrealistic hub-and-spoke recommendations for structuring the continuum of care in underresourced rural contexts. Such recommendations failed to guide providers and offered unfeasible options to vulnerable patients. One participant cynically noted:
Here we are, we’re in the country, we’re gonna tell people, “Guess what? Opioids are bad for you. We know you have problems. Good luck with those. You should get help. Here are a couple of places in the community you can go check out. . . . They probably don’t [take your insurance] and they’re booked out 6 months, but you should do something about that.” That is leaving both us and the patient in a position of great powerlessness.
With shortages in in-house behavioral health resources, many primary care providers relied on referrals in order to intensify care. Yet most participants commented on the long waitlists at county behavioral health departments. “Psychiatric services in this county are not available,” said one physician. “Unless you’re actively homicidal or suicidal, the county psychiatric [unit] will not see a patient.” In one county, participants noted that the inpatient hospitalization services were so poor they were under state compliance investigation. “[It is] mental health jail, essentially, where they get [expletive] treatment—inadequate, treated like animals, thrown back on the street,” commented a system-level stakeholder. “And then they’re back again in 48 hours.” Some participants reported that mental health services would not accept patients who use drugs, because “mental health is so booked up.” In other counties, participants granted that their patients could receive services after a 2- to 3-month wait, but after acute care, services would drop off.
Impacts of the waitlist on patients.
Although people in danger of immediate harm were served, participants argued that waitlists shut people out at the critical moment when they were ready to seek care. One stakeholder explained, “When you’re talking about somebody that’s got withdrawal symptoms plus additional mental health issues, then they can’t just make an appointment in a month and [you can’t] expect them to just show up just fine.” This deficit left a substantial gap in care for anyone with mild to moderate mental health issues, leading many patients to use drugs in the absence of other resources. A deeper consequence, one advocate warned, was that waiting broke people’s trust with health care providers, making it hard for them to consider seeking care again: “[People who use drugs] have spent their entire lives being let down, turned away, talked down to, and you can’t blame somebody for being, ‘You know what? Nope, never mind. They ain’t going to help me. I just can’t do that.’”
Ethically, this approach placed rural providers in a challenging situation, wanting to tackle the deep needs in their communities but understanding the risk factors for burnout inherent in meeting those needs. “I’m just not okay with that system,” explained one therapist, referring to the immense unmet need. “I can’t see 80 clients a week. I have 50 right now.” The risk of burnout only further intensified staffing shortages, because these jobs provided less remuneration and presented intensive demands.
Barriers to private community providers.
Several participants commented that more private practitioners were accepting Medicaid, expanding the psychosocial options. Primary care providers appreciated this expansion because many patients desired more intensive mental health support than they were able to offer. “But here’s the key,” one case manager qualified. “You have to find one who takes your insurance and is willing to see you and has time to see you.” Some felt that the nature of funding available for behavioral health services resulted in an ill-planned “patchwork.” A need remained for more marriage and family therapists and experts in trauma-informed care. For other types of services, such as inpatient rehab programs addressing detoxification or co-occurring conditions, providers often had to send their patients to other counties, where the patients would be placed on waitlists that prioritized local residents. At times, providers sought out treatment approaches that conflicted with their own (e.g., religious treatment programs that prohibited the use of psychiatric medications) just to keep patients in treatment. Consequently, most organizations concentrated on caring for patients in house, knowing the limitations to this approach.
Greater need among remote rural areas.
Participants who worked in remote communities or in frontier counties identified a deeper level of disparity. One provider noted, “We are on the edge and we have no support and . . . it’s a hard place to live.” Being remote, away from metro areas, was felt to exacerbate provider shortages, financial challenges, and feelings of being forgotten. One advocate commented that initiatives to increase rural behavioral health capacity funneled resources to the existing programs, while “focusing on the people [in rural areas] that have the best access.” Such funding patterns bypassed programs with the expertise and capacity to serve the most remote areas. In frontier regions, administrators had to dedicate large portions of their budgets to transport patients to the clinic, because public transportation in their remote county did not reach most patients. Sometimes the most accessible specialist care was available across county or state lines yet remained inaccessible because of the need to “preauthorize” care across behavioral health systems.
Bifurcated System
Lack of trained professionals for co-occurring conditions.
Many participants commented on the challenge of finding personnel to treat co-occurring conditions. The shortage in adequately trained providers resulted from state-mandated criteria for behavioral health licensing that failed to include training in treatment for substance use. One physician explained, “The mental health counselors that we have access to, many of them really don’t understand addiction and don’t understand how to work with [people addicted to drugs], which is kind of stunning to me.” Attempting to expand their organization’s capacity, one provider described their exasperation with finding personnel who could serve patients with co-occurring conditions: “I just had a counselor refuse to see one of our patients because she was still using. . . . We need people who actually can see substance users.” In some cases, untrained providers would begin a course of care then inappropriately cut patients’ treatment plans short, forwarding them to another stage of care with a separate treatment plan.
Prioritization of substance use in evaluations.
Participants asserted that patients’ substance use was prioritized in care, but treatment for mental health conditions was ignored. “They miss it,” explained one participant. “They’re only seeing the use as the problem.” Both “old-school training” and greater stigma toward drug consumption led to greater recognition of substance use in screening and underdiagnosis of mental health conditions across primary care and specialty care organizations. The greater attention to substance use and underdiagnosis of mental health both had long-term consequences. One mental health provider described shock at the long-standing neglect faced by a patient being cared for who had attention-deficit hyperactivity disorder and had been using drugs since adolescence: “I’m like, ‘What medications are you on? What have they done that works for you?’ And he’s like, ‘I’ve never had an evaluation.’” These failures prevented providers from understanding how patients might use substances to address symptoms of mental health conditions.
Discussion
We found that, even as there have been extensive investments in expanding MOUD in rural areas (43), large barriers to offering integrated behavioral health services continue in primary care settings for rural patients with co-occurring opioid use disorder and mental disorders. Our findings indicate that the robust public health efforts to increase the number of x-waivered providers (16–24) may have eclipsed attention to the mental health services that x-waivered providers count on in their provision of MOUD (44). Our findings add to the literature on gaps in the rural mental health system (33, 45–48). Furthermore, our research innovates on the narrow perspective on treatment for opioid use disorder in rural areas by investigating availability of the critical mental health services needed by the two-thirds of patients with opioid use disorder who have co-occurring mental disorders.
Our study highlights substantial obstacles that patients with co-occurring conditions in rural areas face in accessing integrated mental health services, particularly in county systems and in the community. Using the EPIS conceptual model enabled us to highlight the numerous organizational barriers to implementing integrated stepped care. Rural health care organizations attempted to build integrated care capacity in house by sharing mental health providers between organizations, hiring psychiatrists when possible, and utilizing telemedicine. Their experiences are consistent with broader scholarship describing the challenge of staff retention in rural areas (49) and the persistent implementation barriers to effective telemedicine (50). While providers depended on referrals to facilitate integrated care, they underscored the risk that few referrals result in care (51). Even when patients can access care in community settings, length of care may be limited to periods when patients exhibit acute symptoms and quality may be compromised by high rates of workforce turnover. Waitlists pose great risks to patients by potentially leading them to avoid seeking future care or by increasing their distress in the absence of care (52). These risks are particularly high for people in rural areas who are likely to delay or avoid seeking care because of the high social costs of sharing intimate health issues with a provider they may already know in community life (53). Furthermore, providers risk burnout when they feel that their own system does not have the capacity to support them or their patients (49).
Systemic factors critically limit the provision of rural integrated care for MOUD. All provider participants took part in California’s hub-and-spoke system and commented that this intervention included no financial resources to expand mental health treatment capacity. Although hub-and-spoke models have been touted for their capacity to enable integrated care (15), this system-level intervention has neither expanded the workforce of providers with expertise in co-occurring conditions nor made new investments in the county mental health services that rural MOUD providers rely on. Furthermore, a lack of training for integrated care (54) continues to limit the workforce that rural organizations rely on. For mental health researchers, these barriers are well known. Yet as much as practice guidelines for MOUD repeatedly invoke co-occurring mental health conditions, the systemic factors significantly impeding integrated health are persistently ignored in the calls made by drug and public health researchers to address the opioid epidemic (55, 56). Advocates of MOUD have bemoaned the requirement for drug counseling that has long served as a barrier to MOUD even as it is shown to have mixed or no effects, and, correspondingly, they have pushed for a medication-focused approach (57, 58). Yet such an approach has often inadvertently excluded behavioral treatments, such as for co-occurring disorders. Correspondingly, our findings show the recent expansions of opioid treatment largely fail to include widespread funding and strategies promoting the delivery of integrated care.
Regulatory changes made in the wake of the COVID-19 pandemic to loosen restrictions on the provision of telemedicine and to shift MOUD to a remote modality have decreased transportation barriers and potentially increase access to specialists for rural patients (59). Even with loosened telehealth restrictions, many rural organizations likely will need implementation supports to establish sustainable relationships with remote providers (60), as we depict above, and to create work agreements and safety protocols required by specialist telehealth (61). Rural residents are less likely to have the needed broadband and basic technology for telehealth (62), with rural American Indian communities facing gross exclusions (63). Without systematic federal solutions (64), telehealth for rural residents may be accessed by phone alone, if at all. Because of COVID-19, many rural health care organizations have restricted primary care visits to reduce contagion risks and prioritize medically severe patients, thus steepening the treatment barriers for rural patients with co-occurring disorders (65). These restrictions have inadvertently threatened the very viability of these organizations (66). Advances in open access to telehealth may be lost without supports to ensure the long-term survival of rural health care organizations.
Our study was limited by our inclusion of providers from hub-and-spoke programs and other stakeholders in only one state. Although participants resoundingly commented on the paucity of resources for mental health, California counties actually receive more resources for mental health than other states because of funds raised by the Mental Health Services Act (67). Finally, we did not include the perspectives of people who use drugs. Future studies must include their diverse insights to understand the needs of patients in rural areas, the gaps in integrated care, and the solutions to these unique challenges.
Conclusions
Our study indicates several directions for future research. Although studies have explored the availability of counseling within MOUD care in rural areas (23, 68), the need remains to differentiate types of mental health care available to people with co-occurring conditions in these regions in terms of intervention offered, duration, and who receives care. Our findings indicate that people with mild to moderate conditions are currently left out. Considering the evidence that mild cases increase in severity over time (69, 70), gaps excluding such patients represent a critical missed opportunity. Neglecting such patients fails to address their distress, and the resources required for treatment only increase if their conditions intensify. Identifying chasms between rural primary care providers, private providers, and county mental health systems will provide a road map for the next generation of system-level interventions. Finally, future policy research must interrogate barriers that have persistently excluded integrated expertise from training practices. The first phase of response to the opioid epidemic invested significantly in increasing MOUD availability, and future steps must expand the capacity of mental health systems and create comprehensive supports to facilitate integrated MOUD.
1 : Co-occurring substance use and mental disorders among adults with opioid use disorder . Drug Alcohol Depend 2019 ; 197 : 78 – 82 Crossref, Medline, Google Scholar
2 : American Society of Addiction Medicine (ASAM) National Practice Guideline for the Use of Medications in the Treatment of Addiction Involving Opioid Use . J Addict Med 2015 ; 9 : 358 – 367 Crossref, Medline, Google Scholar
3 Clinical Guidelines for the Use of Buprenorphine in the Treatment of Opioid Addiction. Substance Abuse and Mental Health Services Administration, Center for Substance Abuse Treatment, Rockville, MD, 2004Google Scholar
4 : Implementing dual diagnosis services for clients with severe mental illness . Psychiatr Serv 2001 ; 52 : 469 – 476 Link, Google Scholar
5 : The status of addiction treatment research with co-occurring substance use and psychiatric disorders . J Subst Abuse Treat 2008 ; 34 : 1 – 2 Crossref, Medline, Google Scholar
6 : Integrated versus parallel treatment of co-occurring psychiatric and substance use disorders . J Subst Abuse Treat 2006 ; 30 : 79 – 84 Crossref, Medline, Google Scholar
7 : Behavioral health treatment utilization among individuals with co-occurring opioid use disorder and mental illness: evidence from a national survey . J Subst Abuse Treat 2019 ; 98 : 47 – 52 Crossref, Medline, Google Scholar
8 Results from the 2009 National Survey on Drug Use and Health: Mental Health Findings . Substance Abuse and Mental Health Services Administration , Rockville, MD , 2010 Google Scholar
9 : Dual diagnosis capability in mental health and addiction treatment services: an assessment of programs across multiple state systems . Adm Policy Ment Health 2014 ; 41 : 205 – 214 Crossref, Medline, Google Scholar
10 : Development and initial feasibility of an organizational measure of behavioral health integration in medical care settings . J Subst Abuse Treat 2012 ; 43 : 402 – 409 Crossref, Medline, Google Scholar
11 : A unified model of behavioral health integration in primary care . Acad Psychiatry 2018 ; 42 : 265 – 268 Crossref, Medline, Google Scholar
12 : Integrating mental health and primary care . Prim Care 2007 ; 34 : 571 – 592 Crossref, Medline, Google Scholar
13 : Primary care models for treating opioid use disorders: what actually works? A systematic review . PLoS One 2017 ; 12 :
14 : Office-based opioid treatment with buprenorphine (OBOT-B): statewide implementation of the Massachusetts collaborative care model in community health centers . J Subst Abuse Treat 2016 ; 60 : 6 – 13 Crossref, Medline, Google Scholar
15 : Primary care-based models for the treatment of opioid use disorder: a scoping review . Ann Intern Med 2017 ; 166 : 268 – 278 Crossref, Medline, Google Scholar
16 : Rural and Appalachian disparities in neonatal abstinence syndrome incidence and access to opioid abuse treatment . J Rural Health 2018 ; 34 : 6 – 13 Crossref, Medline, Google Scholar
17 : Prescribing practices of nurse practitioners and physician assistants waivered to prescribe buprenorphine and the barriers they experience prescribing buprenorphine . J Rural Health 2019 ; 37 : 211 – 214
18 : Geographic distribution of providers with a DEA waiver to prescribe buprenorphine for the treatment of opioid use disorder: a 5-year update . J Rural Health 2018 ; 35 : 108 – 112 Crossref, Medline, Google Scholar
19 : Prescribing practices of rural physicians waivered to prescribe buprenorphine . Am J Prev Med 2018 ; 54 ( suppl 3 ): S208 – S214 Crossref, Medline, Google Scholar
20 : The role of primary care in improving access to medication-assisted treatment for rural Medicaid enrollees with opioid use disorder . J Gen Intern Med 2019 ; 34 : 936 – 943 Crossref, Medline, Google Scholar
21 : Buprenorphine therapy for opioid addiction in rural Washington: the experience of the early adopters . J Opioid Manag 2012 ; 8 : 29 – 38 Crossref, Medline, Google Scholar
22 : Medication-assisted opioid treatment prescribers in federally qualified health centers: capacity lags in rural areas . J Rural Health 2018 ; 34 : 14 – 22 Crossref, Medline, Google Scholar
23 : Comparing buprenorphine-prescribing physicians across nonmetropolitan and metropolitan areas in the United States . Ann Fam Med 2019 ; 17 : 212 – 220 Crossref, Medline, Google Scholar
24 : Addressing the rural opioid addiction and overdose crisis through cross-sector collaboration: Little Falls, Minnesota . Am J Public Health 2019 ; 109 : 260 – 262 Crossref, Medline, Google Scholar
25 : Widening rural-urban disparities in youth suicides, United States, 1996—2010 . JAMA Pediatr 2015 ; 169 : 466 – 473 Crossref, Medline, Google Scholar
26 : The epidemic of despair among White Americans: Trends in the leading causes of premature death, 1999–2015 . Am J Public Health 2017 ; 107 : 1541 – 1547 Crossref, Medline, Google Scholar
27 : The 2014 Update of the Rural-Urban Chartbook . Grand Forks, ND , Rural Health Reform Policy Research Center , 2014 . https://ruralhealth.und.edu/projects/health-reform-policy-research-center/pdf/2014-rural-urban-chartbook-update.pdf Google Scholar
28 : Providers’ perceptions of prevalent mental and behavioral health problems: differences and similarities across urban, rural, and frontier areas . J Rural Ment Heal 2014 ; 38 : 36 – 49 Crossref, Google Scholar
29 : Comorbid substance and mental disorders among rural Americans: results from the National Comorbidity Survey . J Affect Disord 2007 ; 99 : 265 – 271 Crossref, Medline, Google Scholar
30 : “Putting band-aids on things that need stitches”: immigration and the landscape of care in rural America . Am Anthropol 2018 ; 120 : 487 – 499
31 : De facto mental health services in the rural south . J Health Care Poor Underserved 1995 ; 6 : 434 – 468 Crossref, Medline, Google Scholar
32 : Relationship constellations and dynamics of low-income rural mothers . Affilia 2004 ; 19 :160–173
33 : Rurality and mental health treatment . Adm Policy Ment Heal 2007 ; 34 : 255 – 267
34 : Mental health treatment seeking patterns and preferences of Appalachian women with depression . Am J Orthopsychiatry 2017 ; 87 : 233 – 241 Crossref, Medline, Google Scholar
35 : Vermont responds to its opioid crisis . Prev Med 2015 ; 80 :10–11Crossref, Medline, Google Scholar
36 : Vermont hub-and-spoke model of care for opioid use disorder: development, implementation, and impact . J Addict Med 2017 ; 11 : 286 – 292 Crossref, Medline, Google Scholar
37 : Purposeful sampling for qualitative data collection and analysis in mixed method implementation research . Adm Policy Ment Health 2015 ; 42 : 533 – 544 Crossref, Medline, Google Scholar
38 : Qualitative methods in implementation research: an introduction . Psychiatry Res 2019 ; 280 :
39 : Systematic review of the exploration, preparation, implementation, sustainment (EPIS) framework . Implement Sci 2019 ; 14 : 1 Crossref, Medline, Google Scholar
40 : Advancing a conceptual model of evidence-based practice implementation in public service sectors . Adm Policy Ment Heal 2011 ; 38 :4–23Google Scholar
41 : System-level factors shaping implementation of “hub and spoke” systems to expand MOUD in rural areas . Subst Abus (Epub ahead of print, Dec 7, 2020)Google Scholar
42 Patton MQ: Qualitative Research and Evaluation Methods: Integrating Theory and Practice, 4th ed. Thousand Oaks, CA, Sage Publishing, 2015Google Scholar
43 : Tracking Federal Funding to Combat the Opioid Crisis . , Washington, DC , 2019 Google Scholar
44 : Why aren’t physicians prescribing more buprenorphine? J Subst Abuse Treat 2017 ; 78 : 1 – 7 Crossref, Medline, Google Scholar
45 : Mental Health and Rural America: 1994-2005 . US Department of Health and Human Services , Washington, DC , 2005 . https://www.ruralhealthresearch.org/mirror/6/657/RuralMentalHealth.pdf Google Scholar
46 : Urban vs rural residence and the prevalence of depression and mood disorder among African American women and non-Hispanic White women . JAMA Psychiatry 2015 ; 72 : 576 – 583 Crossref, Medline, Google Scholar
47 : Prevalence of major depressive episodes in rural women using primary care . J Health Care Poor Underserved 2007 ; 18 : 185 – 202 Crossref, Medline, Google Scholar
48 : State mental health policy: it’s never too late to do it right: lessons from behavioral health reform in New Mexico . Psychiatr Serv 2010 ; 61 : 646 – 648 Link, Google Scholar
49 : “If only someone had told me…”: lessons from rural providers . J Rural Health 2011 ; 27 : 122 – 130 Crossref, Medline, Google Scholar
50 : Telemedicine for mental health in the United States: making progress, still a long way to go . Psychiatr Serv 2020 ; 71 : 197 – 198 Link, Google Scholar
51 : Referral and follow-up after mental health screening in commercially insured adolescents . J Adolesc Health 2014 ; 55 : 17 – 23 Crossref, Medline, Google Scholar
52 : Receipt of addiction treatment after opioid overdose among Medicaid-enrolled adolescents and young adults . JAMA Pediatr 2020 ; 174 :
53 : Steps toward a theory of place effects on drug use: risk, marginality, and opportunity in small and remote California towns . Int J Drug Policy 2020 ; 85 :
54 : Barriers to serving clients with co-occurring disorders in a transformed mental health system . Psychiatr Serv 2015 ; 66 : 547 – 550 Link, Google Scholar
55 : A public health strategy for the opioid crisis . Public Health Rep 2018 ; 133 ( suppl 1 ): 24S – 34S Crossref, Medline, Google Scholar
56 : The prescription opioid and heroin crisis: a public health approach to an epidemic of addiction . Annu Rev Public Health 2015 ; 36 : 559 – 574 Crossref, Medline, Google Scholar
57 : When added to opioid agonist treatment, psychosocial interventions do not further reduce the use of illicit opioids: a comment on Dugosh et al . J Addict Med 2016 ; 10 : 283 – 285 Crossref, Medline, Google Scholar
58 : The next stage of buprenorphine care for opioid use disorder . Ann Intern Med 2018 ; 169 : 628 – 635 Crossref, Medline, Google Scholar
59 : Dancing with danger: ethnographic safety, male bravado, and gang research in Colombia . Qual Res 2018 ; 18 : 342 – 360 Crossref, Google Scholar
60 : Telepsychiatry integration of mental health services into rural primary care settings . Int Rev Psychiatry 2015 ; 27 : 525 – 539 Crossref, Medline, Google Scholar
61 : Best practices in videoconferencing-based telemental health April 2018 . Telemed J E Health 2018 ; 24 : 827 – 832 , 2018 Google Scholar
62 : Association between broadband internet availability and telemedicine use . JAMA Intern Med 2019 ; 179 : 1580 – 1582 Crossref, Medline, Google Scholar
63 : Barriers to telemedicine implementation in Southwest tribal communities during COVID‐19 . J Rural Heal 2021 ; 37 : 239 – 241 Google Scholar
64 Simpson A: Under social distancing, rural regions push for more broadband. Pew Charitable Trusts Stateline Blog, May 14, 2020. https://www.pewtrusts.org/en/research-and-analysis/blogs/stateline/2020/05/14/under-social-distancing-rural-regions-push-for-more-broadband?utm_campaign=2020-05-20+Rundown&utm_medium=email&utm_source=Pew Google Scholar
65 : Preventing suicide in rural communities during the COVID‐19 pandemic . J Rural Heal 2021 ; 37 : 179 – 184 Google Scholar
66 Demboski A: Doctors offices are small businesses too. And they’re struggling to stay afloat during the pandemic. KQED, April 15, 2020. https://www.kqed.org/news/11812402/doctors-offices-are-small-businesses-too-and-theyre-struggling-to-stay-afloat-during-the-pandemic Google Scholar
67 : Mental Health Services Oversight and Accountability Commission Evaluation Master Plan . Mental Health Services Oversight and Accountability Commission , Sacramento, CA , 2013 Google Scholar
68 : Perceived need and availability of psychosocial interventions across buprenorphine prescriber specialties . Addict Behav 2019 ; 93 : 72 – 77 Crossref, Medline, Google Scholar
69 : Mild disorders should not be eliminated from the DSM-V . Arch Gen Psychiatry 2003 ; 60 : 1117 – 1122 Crossref, Medline, Google Scholar
70 : Prevalence, correlates, and course of minor depression and major depression in the National Comorbidity Survey . J Affect Disord 1997 ; 45 : 19 – 30 Crossref, Medline, Google Scholar



