Use of Health Care Services Before and After a Natural Disaster Among Survivors With and Without PTSD
Abstract
Objective
This study used a questionnaire to identify individuals who met criteria for posttraumatic stress disorder (PTSD) ten months after surviving a disaster and compared their use of health care services before and after the disaster with that of survivors who did not meet criteria for PTSD.
Methods
Ten months after the December 26, 2004, Southeast Asian tsunami, Danish tourists who had been in areas exposed to the disaster were mailed a questionnaire asking about demographic characteristics and exposure to the tsunami. The questionnaire included the PTSD Checklist, which measures symptoms of posttraumatic stress. Individuals who met DSM-IV PTSD criterion A1—in this case, being caught, touched, or chased by the waves or having witnessed the death, serious injury, or suffering of others—were included in the analyses (N=635). The Danish National Health Service Register provided longitudinal data on annual number of contacts with health care services before (2002–2004) and after (2005–2007) the tsunami.
Results
Survivors with PTSD or partial PTSD used health care services more than survivors without PTSD before and after the tsunami. The severity of posttraumatic stress symptoms was positively correlated with postdisaster use of health care services. However, when adjusted for predisaster health care use, this association was not significant.
Conclusions
Postdisaster health care service utilization was predicted by predisaster health care service utilization and was hardly affected by the onset of PTSD itself. Associations between PTSD and subsequent health problems must be interpreted with caution.
Posttraumatic stress disorder (PTSD) is associated with increased utilization of mental health care and general medical care services (1,2). The greater use of treatment among persons with PTSD may be explained by the need to treat the disorder, but it may be due to associations between PTSD and other mental and general medical disorders (3–5). For example, PTSD is strongly associated with depression, anxiety disorders, somatization, and substance use disorder (6,7). Also, PTSD is associated with hypertension, hyperlipidemia, obesity, and coronary heart disease (8–11).
Most posttraumatic stress research uses cross-sectional or quasiprospective study designs. Indeed, often data are collected after people have been exposed to trauma and sometimes even after people have developed PTSD (12). This is problematic because neither trauma experiences nor the magnitude of posttraumatic stress reactions is randomly distributed in a population. Thus it is often difficult to determine whether associations between PTSD and other mental or general medical disorders or between PTSD and increased health care service utilization are due to trauma exposure, subsequent PTSD symptoms, or preexisting personal, social, and behavioral factors (1,2,12).
This study used both a prospective- and a retrospective-cohort design to investigate associations between PTSD symptoms and the utilization of health care services outside hospitals before and after the 2004 tsunami in Southeast Asia. Our data consisted of the Danish National Health Service Register (NHSR) (13) as well as questionnaires completed ten months after the disaster by a community sample of Danish tourists who experienced the tsunami (14). We examined whether health care service utilization before and after the disaster differed among survivors with PTSD and those without PTSD. We also examined whether the severity of PTSD symptoms ten months after the disaster was related to more frequent use of health care services after the disaster.
Methods
Participants and questionnaire
The participants in this study were Danish tourists who were repatriated from regions affected by the 2004 Southeast Asian tsunami within one or two weeks of the disaster. Upon the survivors’ arrival in Denmark, the police registered their names and personal identification numbers. In total, 2,271 Danes above the age of 18 who potentially had been exposed to the disaster were registered. In November 2005, ten months after the disaster, our questionnaire was mailed to the homes of all the registered survivors who were traceable in the Danish civil registration system (N=2,178) (15). The study was approved by the Danish Data Protection Agency. Ethical approval is not required for this kind of study in Denmark.
The questionnaire asked about demographic variables, exposure to the tsunami, and current symptoms of posttraumatic stress. We asked about specific details regarding disaster exposure, such as whether the participants were caught, touched, or chased by the waves and whether they had witnessed the death, serious injury, or suffering of others (15).
The response rate was 48% (N=1,051). Because of geographic differences in the impact of the tsunami, individuals who were present in Southeast Asia experienced a wide range of exposure (14,16). Therefore, our sample included individuals who had no direct exposure to the tsunami (15). Thus we limited our analysis to those who fulfilled DSM-IV PTSD criterion A1 (17), meaning being caught, touched, or chased by the waves or having witnessed the death, serious injury, or suffering of others. We excluded 362 individuals who did not meet criterion A1 and 54 participants with missing data on outcome variables, leaving 635 participants eligible for the analysis.
The mean±SD age of the study participants was 43.2±12.7 years (range 18–82 years), 51% (N=322) were women, 68% (N=429) were married or cohabiting, 35% (N=223) had completed more than 15 years of education, and 73% (N=465) were employed. The participants were similar to the age-adjusted Danish population in levels of employment (www.statbank.dk/AKU22) and education (www.oecd.org/edu/eag2009). Still, they were more likely to be married or cohabiting (www.statbank.dk/FAM100N).
We assessed posttraumatic stress symptoms with the PTSD Checklist (PCL) (18,19), a well-validated and reliable measure of the 17 PTSD symptoms listed in DSM-IV. The PCL assesses the intensity of PTSD symptoms during the previous month on a 5-point Likert scale, from 1, not at all, to 5, extremely. We used the PCL Stressor Specific Version with instructions to endorse only symptoms linked to tsunami experiences. We considered an item score of 3 or higher to indicate the presence of a particular symptom. This cutoff score is recommended by the National Center for PTSD (www.ptsd.va.gov/professional/pages/assessments/ptsd-checklist.asp). According to DSM-IV criteria, the diagnosis of PTSD requires at least one of five intrusion symptoms from criterion B, three of seven avoidance or numbing symptoms from criterion C, and two of five hyperarousal symptoms from criterion D. We allocated participants into three groups: PTSD, which consisted of participants whose symptoms met DSM-IV criteria for symptom clusters B, C, and D; partial PTSD, which consisted of participants with at least one symptom each from symptom clusters B, C, and D (20,21); and no PTSD, which comprised the remaining participants, who served as the comparison group. PTSD symptom severity was derived from the PCL sum score (possible range 17–85).
National register data
The tsunami occurred on December 26, 2004. We used the NHSR (13) to provide data on the participants’ annual number of contacts with health care services outside hospitals during the three calendar years before the disaster (2002–2004) and during the three calendar years after the disaster (2005–2007). The NHSR was established by Danish authorities, who use it to administer national health insurance for health care services offered outside hospital inpatient and outpatient clinics. All Danish citizens except conscripts, individuals living in institutions, and individuals living abroad are insured by the national health insurance system, and the registry is assumed to be a valid tool for health care research (13). The registry includes all contacts by Danish citizens with general practitioners (GPs), psychologists, psychiatrists, and members of other medical specialties, including physiotherapists, chiropractors, and podiatrists, who offer health care services in the health care sector outside Denmark’s hospitals. The contact dates are specified by week and year. Health care service contacts included consultations, group consultations, e-mail consultations, phone consultations, home visits, individual psychotherapy, and group psychotherapy. Contacts with a preventive purpose and contacts concerning pregnancy care, birth control, and general vaccination programs were excluded from our analysis.
Statistical analysis
We performed chi square tests (linear by linear association) to compare gender, education, marital status, and disaster exposure among participants with PTSD, partial PTSD, and no PTSD. We performed one-way analyses of variance (ANOVAs) with Bonferroni-corrected post hoc t tests to compare health care service utilization before and after the disaster, change in health care service utilization, and age among participants with PTSD, partial PTSD, and no PTSD. The distribution of these variables was found to be sufficiently close to the normal distribution for such analyses (22). Further, we used paired t tests to compare use of health care service before and after the disaster.
We examined the association between predisaster use of health care and postdisaster PTSD by comparing the prevalence of PTSD and partial PTSD and the severity of posttraumatic stress symptoms among participants grouped into quartiles of predisaster health care service contacts. Prevalence was compared by chi square test (linear by linear), and symptom severity was compared by one-way ANOVA.
Finally, the association between severity of posttraumatic stress symptoms ten months after the disaster (November 2005) and the subsequent annual number of contacts with health care services in 2006–2007 was analyzed by linear regression analysis, adjusted for demographic variables and predisaster health care service use. We used the Statistical Package for Social Sciences, version 14.0, for all analyses.
Results
According to their PCL scores, 79 (12%) of the 635 participants fulfilled the DSM-IV symptom criteria B, C, and D for PTSD. In addition, 97 (15%) participants fulfilled our criteria for partial PTSD. Table 1 shows demographic characteristics and tsunami exposure among participants with PTSD, partial PTSD, and no PTSD. Participants with PTSD and partial PTSD included a higher proportion of women, were less likely to be married or cohabiting, and reported more severe exposure to the tsunami than participants without PTSD.
| Characteristic | PTSD(N=79) | Partial PTSD(N=97) | No PTSD(N=459) | |||
|---|---|---|---|---|---|---|
| N | % | N | % | N | % | |
| Female gender | 44 | 55* | 65 | 66 | 213 | 46 |
| Higher education (>15 years) | 23 | 33 | 35 | 40 | 165 | 40 |
| Married or cohabiting | 41 | 53* | 62 | 65 | 326 | 72 |
| Age (M±SD) | 43±13 | 42±14 | 44±13 | |||
| Tsunami exposure | ||||||
| Caught, touched, or chased by the waves | 52 | 66** | 55 | 57 | 191 | 42 |
| Serious injuries inflicted | 7 | 9* | 4 | 4 | 8 | 2 |
| Witnessed deaths or dead bodies | 53 | 67** | 67 | 69 | 220 | 48 |
| Witnessed serious injuries or suffering of others | 62 | 79 | 76 | 78 | 325 | 71 |
| Loss of family member | 8 | 10** | 6 | 6 | 9 | 2 |
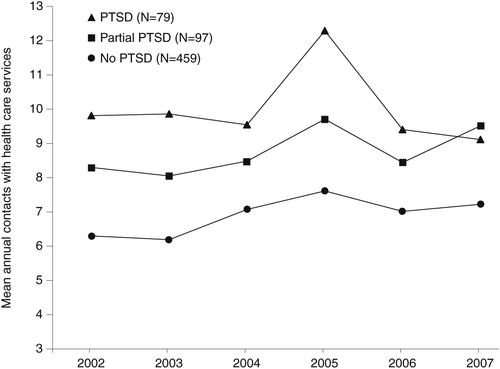
Figure 1 shows the annual number of contacts with health care services before and after the tsunami among participants with PTSD, partial PTSD, or no PTSD. Compared with participants with no PTSD, participants with PTSD or partial PTSD had significantly more annual contacts during the three-year periods before and after the tsunami (Table 2). Annual contacts before and after the tsunami among participants with PTSD and partial PTSD did not differ significantly. Overall, the annual number of contacts with health care services increased .76 (9%) during the three years after the disaster compared with the three years before the disaster (t=4.19, p<.001). The increase in annual contacts for all health care services did not differ among the groups (Table 2).
| Predisaster (2002–2004) | Postdisaster (2005–2007) | Predisaster-postdisaster change | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| PTSD | Partial PTSD | No PTSD | PTSD | Partial PTSD | No PTSD | PTSD | Partial PTSD | No PTSD | ||||||||||
| Service | M | SD | M | SD | M | SD | M | SD | M | SD | M | SD | M | SD | M | SD | M | SD |
| All | 9.7*** | 6.8 | 8.3* | 7.5 | 6.5 | 5.3 | 10.3*** | 6.8 | 9.2* | 6.4 | 7.3 | 5.7 | .5 | 5.3 | .9 | 5.4 | .8 | 4.2 |
| General practitioner | 7.5*** | 5.2 | 6.6* | 6.0 | 5.1 | 4.2 | 8.0*** | 5.2 | 7.1* | 5.1 | 5.6 | 4.5 | .5 | 3.7 | .5 | 4.4 | .5 | 3.5 |
| Psychiatrist | .08 | .6 | .01 | .1 | .02 | .3 | .09** | .6 | .03 | .3 | .04 | .4 | .01 | .7 | .02 | .3 | –.02 | .2 |
| Psychologist | .02 | .2 | .01 | .1 | .02 | .1 | .2** | .6 | .2** | .7 | .05 | .3 | .2** | .6 | .2** | .6 | .04 | .3 |
| Member of other medical specialty | 2.2** | 2.3 | 1.7 | 2.2 | 1.4 | 1.9 | 1.9 | 2.4 | 1.9 | 2.4 | 1.6 | 2.1 | –.2 | 2.4 | .2 | 2.1 | .2 | 1.6 |
The increase in annual contacts with health care services was most prominent during 2005, the year after the disaster (Figure 1). We performed post hoc tests to examine whether there were differences among the groups in the extent to which health care service contacts increased from the three years before the disaster to 2005. The annual number of health care service contacts increased by 2.55 (26%) in the group with PTSD (t=3.54, p<.01), by 1.43 (17%) in the group with partial PTSD, and by 1.09 (17%) in the group with no PTSD (t=4.13, p<.001). The increase in health care service utilization did not differ significantly among the groups.
Table 2 shows that GP contacts constituted a majority of health care service contacts among all groups. Contacts with GPs varied more among the groups than visits for any other health care service. Contacts with psychologists, psychiatrists, and members of other medical specialties constituted only a minor part of the total use of health care services. Overall, contacts with GPs (t=3.34, p<.001), psychologists (t=5.03, p<.001), and members of other medical specialties (t=2.28, p<.05) showed a significant increase after the disaster (Table 2). Use of a psychologist was the only health care service that increased significantly more after the disaster among participants with PTSD and partial PTSD than among participants with no PTSD (F=10.96, p=.001), but even among participants with PTSD and partial PTSD the increase was rather small (.2±.6 contacts).
Table 3 shows the association between predisaster use of health care services and prevalence of postdisaster PTSD and partial PTSD and severity of posttraumatic stress symptoms. The prevalence of PTSD was considerably higher in the quartile with the highest number of predisaster health care service contacts (19%) compared with the quartile with the lowest number of health care service contacts (6%). Also, the severity of posttraumatic stress symptoms was significantly associated with predisaster use of health care services.
| Contacts | ||||||||
|---|---|---|---|---|---|---|---|---|
| ≤3.0(N=159) | 3.1–5.7(N=166) | 5.8–9.3(N=143) | >9.4(N=167) | |||||
| Diagnosis | N | % | N | % | N | % | N | % |
| PTSD | 9 | 6 | 19 | 11 | 20 | 14 | 31 | 19* |
| Partial PTSD | 19 | 12 | 26 | 16 | 24 | 17 | 28 | 17 |
| No PTSD | 131 | 82 | 121 | 73 | 99 | 69 | 108 | 65 |
| PCL scoreb | 26.2 | 24.5–27.9 | 29.9 | 28.0–31.9 | 31.0 | 28.9–33.2 | 34.0 | 31.6–36.4* |
Table 4 shows the association between severity of posttraumatic stress symptoms ten months after the disaster and the annual number of contacts with health care services in 2006–2007. In bivariate analysis, symptom severity was significantly associated with subsequent use of health care services (model 1). The association remained significant when the analysis was adjusted for sociodemographic variables (model 2). When adjusted for predisaster use of health care services, however, the association between severity of posttraumatic stress symptoms and subsequent use of health care services disappeared (model 3).
| Model 1a | Model 2b | Model 3c | ||||
|---|---|---|---|---|---|---|
| Characteristic | β | 95% CI | β | 95% CI | β | 95% CI |
| PTSD Checklist score | .09** | .05 to .12 | .06* | .03 to .10 | .01 | –.02 to .04 |
| Age | .10** | .06 to .14 | .05* | .02 to .08 | ||
| Gender | 3.18** | 2.20 to 4.16 | 1.18* | .36 to 2.00 | ||
| Higher education (>15 years) | –.52 | –1.50 to .46 | –.04 | –.83 to .75 | ||
| Married or cohabiting | –1.94** | –3.01 to .87 | – .74 | 1.62 to .13 | ||
| Predisaster health care service utilization | .62** | .55 to .69 | ||||
Discussion
In our study of a sample of Danish tourists who experienced the Southeast Asian tsunami in 2004, unadjusted analyses showed a relatively strong association between PTSD, partial PTSD, and severity of posttraumatic stress symptoms and use of health care services outside hospitals after the disaster. However, participants with PTSD and partial PTSD had used health care services before the tsunami more frequently than participants with no PTSD. Also, the increase in health care service use before and after the disaster was not significantly higher among participants with PTSD or partial PTSD compared with those with no PTSD. When predisaster use of health care services was taken into consideration, the association between severity of posttraumatic stress symptoms and subsequent use of health care services disappeared.
The ten-month prevalence of PTSD (12%) among survivors who fulfilled DSM-IV PTSD criterion A1 (severely disaster exposed) is consistent with similar reports in the literature (23). The level of health care service utilization by all participants was consistent with rates of utilization in the general Danish population (www.sst.dk/publ/tidsskrifter/nyetal/pdf/2005/02_05.pdf [in Danish]). Also, the finding that PTSD, partial PTSD, and severity of posttraumatic stress symptoms were associated with higher use of health care services is in concert with previous research involving community samples (24), combat veterans (3,5), residents of New York City after the World Trade Center disaster (25), survivors of other man-made (26) and natural disasters (27), and even Scandinavian survivors of the 2004 tsunami (28).
To our knowledge, the association between PTSD and subsequent use of health care services has not previously been adjusted for preexisting use of health care services. Our finding that postdisaster health care service utilization was largely predicted by predisaster health care service utilization and that it was hardly affected by the onset of posttraumatic stress symptoms itself raises important questions about the consequences of traumatic stress, especially from a long-term perspective.
First, our findings prompt questions about previous assertions that the presence of PTSD is the causal factor leading to high health care service utilization (2,29), particularly after one or more years have passed since the trauma. Another alternative explanation is that survivors with PTSD have higher use of health care services even before symptom onset and that PTSD symptoms themselves are not responsible for health care service utilization. Survivors with PTSD may neglect seeking help for their posttraumatic stress (25,30), they may have limited access to adequate treatment in the health care system (31), or their help seeking may replace, or be integrated into, health care consultations they would otherwise carry out. However, neglect of symptoms or limited access to health care was not supported by self-reports of health seeking in the Danish tsunami cohort. For example, ten months after the disaster, 40% of the repatriated Danish tourists, including those who had not been exposed to the tsunami, reported having consulted with their general practitioner for disaster-related problems (28). This treatment-seeking behavior was strongly associated with posttraumatic stress. It is possible, however, that treatment seeking for PTSD may have been strongly limited in the number of consultations and primarily occurred in the close aftermath of the disaster.
Second, our findings raise questions about previous assertions that psychological trauma explains the association between PTSD and other mental and general medical conditions (32). An alternative explanation is that survivors who develop PTSD have a preexisting vulnerability for mental and general medical conditions (33), as suggested by the higher use of health care services before the tsunami. Evidence for this hypothesis includes prospective studies that have identified preexisting mental and general medical conditions (34), neuroticism (35,36) and low cognitive ability (37) as risk factors for PTSD. Thus the frequent use of health care services among individuals with PTSD, as well as their increased vulnerability for other mental and general medical disorders, may be primarily a result of preexisting health conditions, low cognitive functioning, and ineffective coping strategies.
Virtually the entire population of Danes who were in Southeast Asia during the 2004 tsunami was asked to participate in our study, reducing sample selection bias. Furthermore, the Danish population is serviced by national health care that provides relatively equal access to care. Therefore, it is possible to evaluate the relation between PTSD and health care service utilization without considering economic factors. In nations with multipayer health incurrence, based on a mixture of public and private insurance programs, the role of economic factors in use of health care services could not be ignored.
Limitations of the study included a relatively low response rate. However, according to a study of nonresponders in a comparable cohort of Norwegian tsunami survivors who had a similar response rate (38), nonresponders were less likely than responders to have been in a place directly affected by the tsunami and to have fulfilled DSM-IV PTSD criterion A1. Furthermore, in this study, responders and nonresponders were similar with regard to age (15) and predisaster use of health care outside hospitals. Also, participants were similar to the general Danish population with regard to education and employment and included women and men of all ages.
Whether participants fulfilled DSM-IV PTSD criterion A1 was assessed by retrospective self-report, which may have been distorted by memory bias (39). To minimize such bias, we defined exposure on the basis of what may be considered objective events. The use of a single, self-report questionnaire to measure participants’ symptoms ten months after the disaster was also a limitation. Although the PCL is based on the DSM-IV symptom criteria, it cannot substitute for more comprehensive clinical interviews.
Our use of prospective national register data provided a measure of health care service utilization outside hospitals that is unaffected by possible recall and information biases that typically influence self-reports. Also, the equal accessibility of commonly acknowledged treatment minimized possible selection biases. The use of GPs is a sensitive measure of individual use of both social and health care services, given that the GP is a gatekeeper to other health care services as well as the physician who bears responsibility for communicating to social authorities.
Another limitation was entering utilization of health care services in the second and third years after the disaster as a variable in our predictive regression model. During this time frame, some survivors may have recovered from PTSD, resulting in reduced health care use. However, epidemiological research suggests that one-third of individuals who develop acute PTSD remain symptomatic for six years or longer (6). Similarly, 43% of the Danish tsunami survivors who had PTSD or partial PTSD ten months after the disaster were still symptomatic during a follow-up survey conducted two-and-one-half years after the disaster, indicating that a majority still suffered from disaster-related health problems (40).
Conclusions
This study found that postdisaster health care service utilization was predicted by predisaster health care service utilization and was hardly affected by the onset of PTSD itself. Our findings underline the importance of considering antecedents to trauma exposure when addressing the association between PTSD and health care service utilization. Similar considerations may also have consequences for the interpretation of the relationship between PTSD and later onset of comorbid disorders. The absence of important historical or pretrauma information may be a serious limitation within posttraumatic stress research.
1 : Use of mental health services among disaster survivors. Current Opinion in Psychiatry 21:370–378, 2008Crossref, Medline, Google Scholar
2 : Health service use predictors among trauma survivors: a critical review. Psychological Services 2:3–19, 2005Crossref, Google Scholar
3 : PTSD and utilization of medical treatment services among male Vietnam veterans. Journal of Nervous and Mental Disease 188:496–504, 2000Crossref, Medline, Google Scholar
4 : Health status, somatization, and severity of posttraumatic stress disorder in Vietnam combat veterans with posttraumatic stress disorder. American Journal of Psychiatry 155:1565–1569, 1998Link, Google Scholar
5 : Posttraumatic stress disorder and the use of health services. Psychosomatic Medicine 63:835–841, 2001Crossref, Medline, Google Scholar
6 : Posttraumatic stress disorder in the National Comorbidity Survey. Archives of General Psychiatry 52:1048–1060, 1995Crossref, Medline, Google Scholar
7 : Comorbidity of psychiatric disorders and posttraumatic stress disorder. Journal of Clinical Psychiatry 61(suppl 7):22–32, 2000Crossref, Medline, Google Scholar
8 : A prospective study of PTSD and early-age heart disease mortality among Vietnam veterans: implications for surveillance and prevention. Psychosomatic Medicine 70:668–676, 2008Crossref, Medline, Google Scholar
9 : Hypertension in relation to posttraumatic stress disorder and depression in the US National Comorbidity Survey. Behavioral Medicine 34:125–132, 2009Crossref, Medline, Google Scholar
10 : Abnormal serum lipid profile in Brazilian police officers with posttraumatic stress disorder. Journal of Affective Disorders 107:259–263, 2008Crossref, Medline, Google Scholar
11 : Obesity and mental disorders in the adult general population. Journal of Psychosomatic Research 64:97–105, 2008Crossref, Medline, Google Scholar
12 : Progress and controversy in the study of posttraumatic stress disorder. Annual Review of Psychology 54:229–252, 2003Crossref, Medline, Google Scholar
13 : The Danish National Health Service Register: a tool for primary health care research. Danish Medical Bulletin 44:449–453, 1997Medline, Google Scholar
14 : Exposure characteristics and peri-trauma emotional reactions during the 2004 Southeast Asian tsunami: what predicts posttraumatic stress and depressive reactions? Comprehensive Psychiatry 52:630–637, 2011Crossref, Medline, Google Scholar
15 : Tsunami-affected Scandinavian tourists: disaster exposure and posttraumatic stress symptoms. Nordic Journal of Psychiatry 65:9–15, 2011Crossref, Medline, Google Scholar
16 : Acute disaster exposure and mental health complaints of Norwegian tsunami survivors six months post disaster. Psychiatry 71:266–276, 2008Crossref, Medline, Google Scholar
17 Diagnostic and Statistical Manual of Mental Disorders, 4th ed. Washington, DC, American Psychiatric Association, 1994Google Scholar
18 Weathers F, Litz B, Herman D, et al: The PTSD Checklist (PCL): reliability, validity, and diagnostic utility. Presented at the annual meeting of the International Society for Traumatic Stress Studies, San Antonio, Tex, Oct 1993. Available at www.pdhealth.mil/clinicians/assessment_tools.asp#ptsdcGoogle Scholar
19 : The Norwegian version of the PTSD Checklist (PCL): construct validity in a community sample of 2004 tsunami survivors. Nordic Journal of Psychiatry 66:355–359, 2012Crossref, Medline, Google Scholar
20 : Full and partial posttraumatic stress disorder: findings from a community survey. American Journal of Psychiatry 154:1114–1119, 1997Link, Google Scholar
21 : Partial PTSD versus full PTSD: an empirical examination of associated impairment. Psychological Medicine 34:1205–1214, 2004Crossref, Medline, Google Scholar
22 : Performance of five two-sample location tests for skewed distributions with unequal variances. Contemporary Clinical Trials 30:490–496, 2009Crossref, Medline, Google Scholar
23 : Posttraumatic stress disorder following disasters: a systematic review. Psychological Medicine 38:467–480, 2008Crossref, Medline, Google Scholar
24 : Functional impairment and utilization of services associated with posttraumatic stress in the community. Journal of Traumatic Stress 12:709–724, 1999Crossref, Medline, Google Scholar
25 : Disparities in mental health treatment following the World Trade Center disaster: implications for mental health care and health services research. Journal of Traumatic Stress 18:287–297, 2005Crossref, Medline, Google Scholar
26 : Correlates of mental health services utilization 18 months and almost 4 years postdisaster among adults with mental health problems. Journal of Traumatic Stress 20:1029–1039, 2007Crossref, Medline, Google Scholar
27 : PTSD, depression and help-seeking patterns following the Miyake Island volcanic eruption. International Journal of Emergency Mental Health 4:157–171, 2002Medline, Google Scholar
28 : Use of and satisfaction with support received among survivors from three Scandinavian countries after the 2004 Southeast Asian tsunami. European Psychiatry 26:436–440, 2011Crossref, Medline, Google Scholar
29 : Correlates of mental health service use intensity in the National Comorbidity Survey and National Comorbidity Survey Replication. Psychiatric Services 58:1108–1115, 2007Link, Google Scholar
30 : Was there unmet mental health need after the September 11, 2001, terrorist attacks? Social Psychiatry and Psychiatric Epidemiology 41:230–240, 2006Crossref, Medline, Google Scholar
31 : Mental health treatment received by primary care patients with posttraumatic stress disorder. Journal of Clinical Psychiatry 64:1230–1236, 2003Crossref, Medline, Google Scholar
32 : The long-term costs of traumatic stress: intertwined physical and psychological consequences. World Psychiatry 9:3–10, 2010Crossref, Medline, Google Scholar
33 : Psychosocial and health belief variables associated with frequent attendance in primary care. Psychological Medicine 29:1347–1357, 1999Crossref, Medline, Google Scholar
34 : Baseline self-reported functional health and vulnerability to posttraumatic stress disorder after combat deployment: prospective US military cohort study. BMJ 338:b1273, 2009Crossref, Medline, Google Scholar
35 : Do personality traits predict post-traumatic stress? A prospective study in civilians experiencing air attacks. Psychological Medicine 35:659–663, 2005Crossref, Medline, Google Scholar
36 : Premilitary MMPI scores as predictors of combat-related PTSD symptoms. American Journal of Psychiatry 150:479–483, 1993Link, Google Scholar
37 : Pretrauma cognitive ability and risk for posttraumatic stress disorder: a twin study. Archives of General Psychiatry 64:361–368, 2007Crossref, Medline, Google Scholar
38 : Nonresponse to a population-based postdisaster postal questionnaire study. Journal of Traumatic Stress 22:324–328, 2009Crossref, Medline, Google Scholar
39 : Longitudinal changes in recalled perceived life threat after a natural disaster. British Journal of Psychiatry 194:510–514, 2009Crossref, Medline, Google Scholar
40 Rosendal S: Disaster exposure, posttraumatic stress symptoms, and use of health care services: an epidemiological study of the Danish tsunami cohort. Doctoral thesis, Psychiatric Centre Copenhagen and University of Copenhagen, Centre for Crisis and Disaster Psychiatry, 2011Google Scholar



