Outcomes of Poorly Functioning Patients With Personality Disorders in a Day Treatment Program
Abstract
OBJECTIVE: Rates of completion, complications, and outcome were examined in a sample of poorly functioning patients who participated in a group-oriented day treatment program for patients with personality disorders. METHODS: The study was a naturalistic prospective study of 183 patients admitted to a day treatment program in Oslo, Norway. The program consists of a combination of group analytically oriented groups and cognitive-behavioral groups. The Global Severity Index (GSI) of the Symptom Check List, the circumplex version of the Inventory of Interpersonal Problems (IIP-C), and the Global Assessment of Functioning (GAF) were administered at admission and discharge. RESULTS: A total of 141 patients (77 percent) completed the day treatment program. Few patients experienced treatment complications. Effect sizes for GAF, GSI, and IIP-C scores for treatment completers were in the medium-to-high range, indicating a fair level of improvement. Patients' rating of benefit was positive. CONCLUSIONS: The results are promising as a first step toward development of a cost-efficient comprehensive long-term treatment program for patients with severe personality disorders.
Patients with personality disorders are heterogeneous in functional impairment and symptom distress. A substantial number of these patients need more intensive treatment than afforded in ordinary outpatient settings. During the last two decades, interest has increased in partial hospitalization as an alternative to inpatient treatment, partly due to economic considerations (1).
Specialized day or evening treatment programs for selected diagnostic categories have been developed as one kind of partial hospitalization (2, 345678). Compared with inpatient treatment, day treatment programs have the advantages of reduced costs and may prevent regression among patients at risk of severe decompensation (2,9). In the area of personality disorders, the Edmonton day treatment program (7) and the Edmonton evening treatment program (8) are among the most thoroughly described. These 18-week group-oriented treatment programs have been found to be effective.
However, the treatment models are connected to the time-limited format and have included patients who have mainly cluster C personality disorders, or better-functioning patients (8). Patients with severe personality disorders are often characterized by poor relationships, unstable conduct of life, a low level of psychological mindedness and problems with forming a treatment alliance, which make them poor candidates for short-term psychotherapy (10,11). It is commonly accepted that patients with severe personality disorders need longer-term treatment (12,13,14), and recent studies have provided preliminary empirical evidence of this need (15,16,17,18).
The treatment model described in this paper combines the advantages of the time-limited Edmonton model with longer-term follow-up treatment, which may render the model suitable also for more seriously disturbed patients with personality disorders. The treatment model has two phases: a time-limited day treatment program, followed by long-term outpatient group psychotherapy.
The short-term goals of the first phase include starting a therapeutic process by establishing a therapeutic alliance, encouraging the patient's attachment to the treatment program, and motivating the patient for longer-term therapy. Other short-term goals are symptom relief, reduction of acting out, and development of plans for rehabilitation to work, training, or education. The long-term goals of the outpatient group psychotherapy component are rehabilitation and psychological maturation, by the patient's working through intrapsychic and interpersonal conflicts.
This paper focuses on the day treatment phase and describes treatment experiences with poorly functioning patients with personality disorders with special emphasis on dropout rates, attendance, and treatment complications, as well as outcomes.
Methods
The day treatment program
The day treatment program is located at Ullevaring;l University Hospital in Oslo, Norway, and receives patients from the whole city. The day treatment program consists of a combination of group analytically oriented groups (19) and cognitive-behavioral groups. Twenty-four patients are treated during 18 weeks by participation in ten different groups, five days a week, from 9 a.m. until about 2 p.m. The ten groups are the large group, the analytic small group, the art therapy group, the body awareness group, the cognitive group, and the anxiety group, as well as the problem-solving group, the steering group, the medication group, and the daily closing group.
The overall treatment theory is based on a blend of group analysis (19), principles related to therapeutic communities (20), and self psychology (21). The group program was inspired by the Edmonton day treatment program developed by Piper and associates, and the length of the day treatment part was chosen to make the results comparable.
No individual psychotherapy is offered in the day treatment program. An increased need for staff and development of complicated transferences and countertransferences are arguments against combined individual and group therapy in this setting. However, each patient has an administrative therapist who leads the patient through the program and keeps contact with outside professionals. For 15 percent of the 183 patients in the study reported here, the program staff have made some kind of contact with the family, mainly supportive interventions. All groups are co-led by two therapists. The multidisciplinary staff consists of nine professionals. Three are group analysts, and three are currently in group analytic training.
The day treatment program is followed by outpatient group analytic psychotherapy, one and a half hours weekly, with a time limit of three and a half years. In 1998, a total of 11 outpatient groups existed, and the staff is supplemented by six visiting group psychotherapists.
The cost of the total treatment is approximately $12,000 per patient (U.S. dollars): $8,000 for the day treatment program and $4,000 for the outpatient group psychotherapy. The program is run by a nonprofit public hospital, and the estimated costs do not include rent, electricity, taxes, and hospital administration. The patients pay nothing for the day treatment program and a maximum of $170 annually for outpatient group psychotherapy.
Assessments
The study had a naturalistic prospective design. Standardized routines for patient and treatment assessments were an integrated part of the treatment program. All patients completed an application form, covering clinical and sociodemographic information. The therapists completed an additional clinical and treatment data form. The Symptom Check List (SCL- 90-R) (22) and the circumplex version of the Inventory of Interpersonal Problems (IIP-C) (23) were mailed to all subjects before admission. The Global Severity Index (GSI) from the SCL-90-R was used to measure severity of symptoms. These measures were repeated at discharge. At admission the patients were also given a Global Assessment of Functioning (GAF) score (24) on the basis of team consensus. At discharge the patients rated total treatment benefit on a scale from 1 to 7, with 1 indicating no benefit and 7 very much benefit.
The Structured Clinical Interview for DSM-III-R/IV axis I disorders (SCID-I) (25) was administered by two external raters one to two weeks before, or shortly after, admission. Reliability ratings based on a subsample of 40 audiotaped interviews were satisfactory. Kappas for the categories major depression, bipolar disorder, dysthymia, social phobia, panic disorder, obsessive-compulsive disorder, eating disorder, somatoform disorders, and substance abuse or dependence ranged from .78 to 1.
The SCID for DSM-III-R/IV axis II disorders (SCID-II) was administered by the therapists at the beginning of the treatment. After discharge, based on all available information, the SCID-II protocols were revised after team discussions in the presence of two independent researchers. The patients were also given a GAF score by the team at discharge.
Subjects
Before admission, patients signed a form consenting to participate in clinical research. During the period from October 1993 to October 1996, 183 consecutively admitted patients were included in the study. Eighty-two patients (45 percent) were referred from psychiatric outpatient departments; 51 (28 percent) from private psychiatrists, psychologists, or general practitioners; 28 (15 percent) from acute psychiatric wards; and 22 (12 percent) from other settings.
As Table 1 shows, 75 percent of the patients were female. The mean±SD age was 33±8 years. Fifty-three percent had never been married, and 50 percent were living alone. Work functioning was poor for a great majority of the patients. Thirty-two percent had taken from three to 12 months of sick leave in the past year, 35 percent were receiving rehabilitation benefits, and 2 percent were receiving a disability pension. In Norway, patients who receive rehabilitation benefits have been on continuous sick leave for a minimum of one year. Twelve percent of the patients were unemployed at admission. Among the 67 patients (37 percent) who were employed, 58 (87 percent) were on sick leave or were receiving rehabilitation benefits.
As Table 1 shows, many patients had experienced previous psychiatric hospitalizations (43 percent), and nearly all patients had had previous outpatient treatment (96 percent). Previous treatment included a considerable amount of psychotherapy, which was measured as regular psychotherapy at least once a week for at least three months. Forty-two percent of the patients had tried to commit suicide in the past, 27 percent had episodes of self-mutilation, and 37 percent had experienced severe behavioral dyscontrol in the sense of attacking objects or people. Fifty-five percent of the patients were on medication at the time of admission, mainly antidepressants.
Table 2 shows that personality disorders were diagnosed for 159 patients (87 percent). For three patients who dropped out early, axis II diagnoses were deferred. The most frequent personality disorders were borderline (N=70) and avoidant (N=69) personality disorders, followed by personality disorder not otherwise specified (N=32), dependent (N=29), and paranoid (N=17) personality disorder. Because many patients had comorbid personality disorders across clusters, we created a hierarchy of clusters. All patients with a personality disorder in cluster A were categorized as cluster A (13 percent). Patients with a personality disorder in cluster B were categorized as cluster B (31 percent) unless they had a comorbid cluster A personality disorder. Patients were categorized as cluster C (26 percent) when they did not have additional cluster A or B personality disorders.
Table 2 also shows that nearly all patients (N=179, or 98 percent) had current axis I diagnoses.
Data analysis
Differences between groups were tested by independent-sample two-tailed t test, Fisher's exact test, and one-way analysis of variance with Scheffé's procedure. The paired t test was used to test differences in pre- and posttreatment scores. Logistic regression analysis was applied to make a model for prediction of irregular discharge. Due to missing data, the N varies slightly in the tables.
Results
Dropout rates
Forty of the 183 patients (22 percent) were discharged irregularly: 29 patients (16 percent) dropped out, nine patients (5 percent) were discharged for breaking the treatment contract, and two patients (1 percent) were transferred to another ward. Two patients (1 percent) were discharged for other reasons—epileptic seizures and premature termination due to a work offer—and they were excluded from further analyses.
Among the 70 patients with borderline personality disorder, 20 (29 percent) were discharged irregularly. A total of 141 patients (77 percent) completed the day treatment program. The mean±SD length of stay for irregularly discharged patients was 6.5±6.5 weeks, compared with 20.2±3.2 weeks for treatment completers.
Irregularly discharged patients were younger than other patients at admission (31 versus 34 years; t=2.36, df=179, p<.05) and younger at their first contact with psychiatric services (20 versus 25 years; t=2.36, df=153, p<.05). They were more often unskilled in terms of education (53 percent versus 25 percent; χ2=11.17, df= 1, p<.01) and more likely to be unemployed (28 percent versus 8 percent; Fisher's statistic=9.90, df=1, p<.01).
The GAF score at admission was significantly lower for patients who were irregularly discharged (41.4 versus 45.6; t=4.89, df=179, p<.01). Patients with more than two previous suicide attempts were more likely than other patients to be discharged irregularly (33 percent versus 13 percent; N=180; χ2=8.42, df=1, p<.01). Five of the seven patients with antisocial personality disorder were irregularly discharged (Fisher's statistic= 8.32, df=1, p<.01). Irregularly discharged patients had more often misused substances in the month before admission (30 percent versus 11 percent; χ2=8.2, df=1, p<.01). No significant differences between irregularly discharged patients and treatment completers were found in GSI or IIP-C scores at admission.
Several variables were explored in multiple logistic regression analyses, with irregular discharge as the dependent variable. We developed a model for irregular discharge consisting of three variables: GAF score at admission, unskilled in terms of education, and antisocial personality disorder. The odds ratios for irregular discharge were .41 (95 percent confidence interval=.26 to .66, p<.001) for every 5-unit increase in GAF at admission, 2.55 (CI=1.16 to 5.62, p< .05) for being unskilled, and 6.18 (CI=1.09 to 34.98, p<.05) for having an antisocial personality disorder. The specificity of the model was .98, and the sensitivity was .33. Further analyses are reported only for the 141 patients who completed the program.
Attendance
The majority of the patients who completed the program (102 of 139 patients, or 73 percent) attended treatment regularly. Twenty-six patients (19 percent) had some irregular attendance, and for 11 patients (8 percent) irregular attendance represented a serious treatment problem.
Complications
No attacks on people or furniture occurred. Threatening verbal or physical behavior (four patients, or 3 percent) and suicide attempts (two patients, or 1 percent) were rare. Self-mutilation was somewhat more frequent (11 patients, or 8 percent). It was necessary to transfer seven patients (5 percent) temporarily to an acute ward, due to risk of suicide or psychotic regression.
Outcome
Changes in GAF, GSI, and IIP-C scores from pretest to posttest were significant (GAF, t=12.93, df=140, p<.01; GSI, t=6.22, df=140, p<.001; IIP-C, t=6.38, df=140, p<.001; paired t tests). For calculation of effect sizes, we used the prescore standard deviations as a standardization. As shown in Table 3, the effect sizes for treatment completers were generally large for the GAF score and medium for the GSI and IIP-C scores (26). The effect size for the GAF score was largest among the patients who did not have a personality disorder; these patients also had the highest mean GAF score at admission. The effect size for patients with cluster A personality disorders, who had the lowest mean GAF score at admission, was also in the large range. Furthermore, the effect sizes for GSI and IIP-C scores were largest for patients with cluster A personality disorders and patients who did not have a personality disorder.
Ninety-eight patients (70 percent) were treated with psychotropic drugs, mainly antidepressants, during the stay. Patients who were not on medication during the stay had significantly lower GSI scores at discharge than those who received medication (.89 versus 1.25; t=3.21, df=101, p<.01) even though the GSI scores for the two groups did not differ significantly at admission (1.51 and 1.49, respectively). The lower GSI scores at discharge among patients not on medication compared with patients on medication was significant both among patients with mood disorders (.94 versus 1.29; t=2.42, df=110, p<.05) and patients with comorbid mood and anxiety disorders (.87 versus 1.40; t=2.32, df=61, p<.05). No significant difference in personality disorder clusters was found between patients receiving and not receiving medications.
The patients' mean±SD rating of their total benefit from the stay was 5±1.4, which represents a moderate positive benefit. Fifty-seven patients (41 percent) resumed work or studies within three months after discharge, and 75 (54 percent) continued to be on sick leave or to receive rehabilitation benefits.
Discussion
The completion rate in the study reported here is in the same range as those found for the Edmonton evening treatment program (71 percent) (8) and the Edmonton day treatment program (79 percent) (7). The rates for dropout and expulsion are comparable to those found for the Edmonton evening treatment program (a 15 percent dropout rate and a 4 percent expulsion rate). The rate of irregular discharge for patients with borderline personality disorder was in the lower range of rates reported in the literature (27).
The overall positive changes in patients' symptoms and functioning found in this study also replicate the findings for both of the Edmonton programs. The medium-to-high effect sizes of the outcome measures are comparable to the effect size on the IIP in the study of the Edmonton evening treatment program, although the effect sizes for the GAF and GSI were somewhat lower in our study. Furthermore, the posttreatment scores on the GSI, IIP-C, and GAF found in this study are in the range found among outpatients (24,28; Horowitz LM, unpublished manuscript) and are consistent with appropriate placement in outpatient psychotherapy, given a good treatment alliance. However, even though acceptable effect sizes on outcome measures were found for patients with cluster A personality disorders, they had a low level of global functioning at discharge and may have had special needs in follow-up treatment.
The lack of a control group in the study prevents a firm conclusion that the improvements were treatment effects. However, the findings in the Edmonton day treatment program study, which included a control group, point toward a possible treatment effect, as do the findings in the study reported here of change at the group level among patients with such long-standing disorders as personality disorders and the fact that most patients were not in acute crises at admission but had been on a waiting list for several months.
Medication is an integrated part of the day treatment program, and the drug treatment and indications for such treatment were not sufficiently systematized to distinguish between a medication effect and a pure psychotherapy effect. Our finding that patients who were not treated with medication had a better outcome on the GSI is puzzling, but it is in line with previously reported results for a subsample of the patients in this study (29). That study found that many patients with severe personality disorders can be treated by psychodynamic group therapy without additional drug treatment.
A main issue in this study was whether it is possible to extend the indication for a specialized group-oriented day treatment program to patients with more severe personality disorders. Compared with the sample in the Edmonton day treatment study (7), the rates of previous hospitalization were similar to those in our sample. GSI scores were high in both samples (1.5 in this study and 1.4 in the Edmonton study). However, patients' capacity for work and study were lower in our sample; in the Edmonton day treatment program 30 percent of the sample was employed full time. Compared with the sample in the Edmonton day program, our sample comprised more patients with any personality disorder (87 percent versus 62 percent) and with personality disorders in clusters A and B, particularly borderline and paranoid personality disorders. In the Edmonton sample, dependent personality disorder was the largest diagnostic group.
The sample in the study of the Edmonton evening treatment program comprised a substantial number of patients with borderline and paranoid personality disorders (8). On the other hand, one inclusion criterion for the evening program was meaningful activity during the daytime, such as work, training, or education. The Edmonton evening program participants represented the less disturbed end of the spectrum, with a mean admission GAS score of 61 and a GSI score of 1.2. The studies of the Edmonton day and evening programs excluded patients with current substance abuse. Thus the evidence indicates that our sample represented more severely disturbed and poorly functioning patients.
Irregular discharges probably resulted from a complex interaction between patient and treatment characteristics and life circumstances. This study's model for irregular discharge may not be generalizable, due to the explorative nature of the analyses and the small number of patients with antisocial personality disorder. Furthermore, we still have limited knowledge of who will benefit from longer-term treatment among poorly functioning patients with personality disorders. At this point, rather than excluding patients at high risk for dropout, we prefer to include them in anticipation of eventually tailoring the treatment to their needs. Although only 5 percent of patients in our study were temporarily transferred to the acute ward, this proportion probably does not reflect the total need for additional care, because a few more patients spent some nights at the walk-in clinic in the city. However, the overall need for 24-hour care was low.
Conclusions
The acceptable rate of completion, low frequency of complications, and overall positive change found for patients in our day treatment program are promising, considering the efforts to establish more comprehensive cost-efficient treatment programs for patients with severe personality disorders.
At this point, we cannot estimate to what degree the results of the study are related to the expectancies of the second part of the treatment program, the outpatient component. Only the one- and five-year follow-up studies that are integrated into the program will show further developments among these patients—to what degree they succeed in engaging in longer-term psychotherapy and the benefits of the follow-up treatment.
Acknowledgment
This research was funded by Ullevål University Hospital.
The authors are affiliated with the division of psychiatry at Ullevaring;l University Hospital, N-0407 Oslo, Norway [email protected].
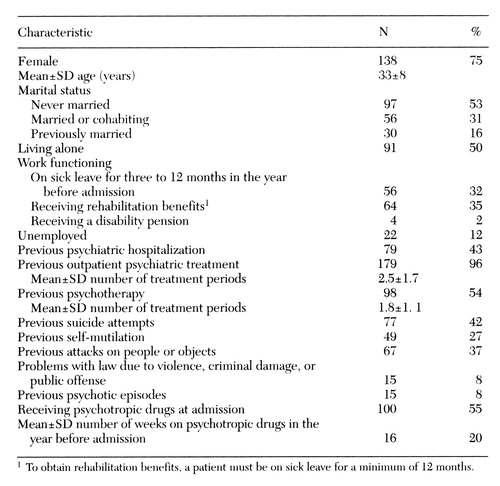 |
Table 1. Sociodemographic and clinical characteristics of 183 participants in a day treatment program for patients with personality disorders
 |
Table 2. DSM-III-R and DSM-IV axis II and axis I diagnoses of 183 participants in a day treatment program for patients with personality disorders
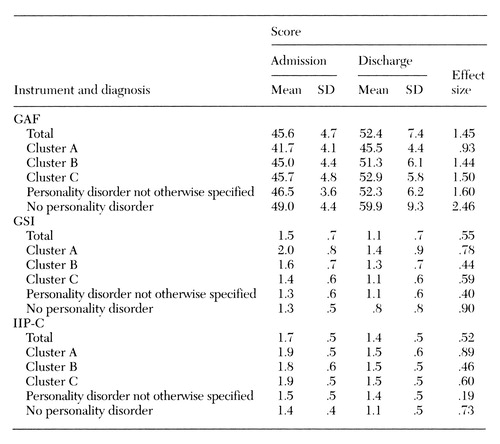 |
Table 3. Scores on the Global Assessment of Functioning (GAF), the Global Severity Index (GSI), and the Inventory of Interpersonal Problems (IIP-C) at admission and discharge and effect size for 141 patients who completed a day treatment program
1. Hoge MA, Davidson L, Hill WL, et al: The promise of partial hospitalization: a reassessment. Hospital and Community Psychiatry 43:345-354, 1992Abstract, Google Scholar
2. Rosie JS, Azim HFA, Piper WE, et al: Effective psychiatric day treatment: historical lessons. Psychiatric Services 46:1019-1026, 1995Link, Google Scholar
3. Karterud S, Vaglum S, Friis S, et al: Day hospital therapeutic community treatment for patients with personality disorders: an empirical evaluation of the containment function. Journal of Nervous and Mental Disease 180:238-243, 1992Crossref, Medline, Google Scholar
4. Sandell R, Alfredsson E, Merg M, et al: Clinical significance of outcome in long-term follow-up of borderline patients at a day hospital. Acta Psychiatrica Scandinavica 87:405-413, 1993Crossref, Medline, Google Scholar
5. Conner KR, Silverstein SM, McCullock Melnyk KA, et al: The development of partial hospitalization program for mentally ill chemically abusing (MICA) patients. Journal of Substance Abuse Treatment 12:311-318, 1995Crossref, Medline, Google Scholar
6. Piper WE, Rosie JS, Azim HFA, et al: A randomized trial of psychiatric day treatment for patients with affective and personality disorders. Hospital and Community Psychiatry 44:757-763, 1993Abstract, Google Scholar
7. Piper WE, Rosie JS, Joyce AS, et al: Time-Limited Day Treatment for Personality Disorders: Integration of Research and Practice in a Group Program. Washington, DC, American Psychological Association, 1996Google Scholar
8. McCallum M, Piper WE, O'Kelly J: Predicting patient benefit from a group-oriented, evening treatment program. International Journal of Group Psychotherapy 47:291-314, 1997Crossref, Medline, Google Scholar
9. Parker S, Knoll JL: Partial hospitalization: an update. American Journal of Psychiatry 147:156-160, 1990Link, Google Scholar
10. Høglend P: Personality disorders and long-term outcome after brief dynamic psychotherapy. Journal of Personality Disorders 7:168-181, 1993Crossref, Google Scholar
11. Piper WE, Joyce AS, Rosie JS, et al: Psychological mindedness, work, and outcome in day treatment. International Journal of Group Psychotherapy 44:291-311, 1994Crossref, Medline, Google Scholar
12. Higgit A, Fonagy P: Psychotherapy in borderline and narcissistic personality disorder. British Journal of Psychiatry 161:23-43, 1992Crossref, Medline, Google Scholar
13. Kernberg O: Severe Personality Disorders: Psychotherapeutic Strategies. New Haven, Conn, Yale University Press, 1984Google Scholar
14. Gunderson JG: Borderline Personality Disorder. Washington DC, American Psychiatric Press, 1984Google Scholar
15. Linehan MM, Armstrong HE, Suarez A, et al: Cognitive-behavioral treatment of chronically parasuicidal borderline patients. Archives of General Psychiatry 48:1060-1064, 1991Crossref, Medline, Google Scholar
16. Linehan MM, Heard HL, Armstrong HE: Naturalistic follow-up of a behavioral treatment for chronically parasuicidal borderline patients. Archives of General Psychiatry 50:971-974, 1993Crossref, Medline, Google Scholar
17. Monsen J, Odland T, Faugli A, et al: Personality disorders and psychosocial changes after intensive psychotherapy: a prospective follow-up study of an outpatient psychotherapy project, 5 years after end of treatment. Scandinavian Journal of Psychology 36:256-268, 1995Crossref, Medline, Google Scholar
18. Mehlum L, Friis S, Irion T, et al: Personality disorders 2-5 years after treatment: a prospective follow-up. Acta Psychiatrica Scandinavica 84:72-77, 1991Crossref, Medline, Google Scholar
19. Foulkes SH, Anthony EJ: Group Psychotherapy: The Psychoanalytic Approach. London, Penguin Books, 1957Google Scholar
20. Karterud S: Community meetings and the therapeutic community, in Comprehensive Group Psychotherapy. Edited by Kaplan HI, Sadock BJ. Baltimore, Williams & Wilkins, 1996Google Scholar
21. Kohut H: How Does Analysis Cure? London, University of Chicago Press, 1984Google Scholar
22. Derogatis LR: The SCL-90: Administration, Scoring, and Procedures Manual-II for the Revised Version. Baltimore, Clinical Psychometric Research, 1977Google Scholar
23. Alden LE, Wiggins JS, Pincus AL: Construction of circumplex scales for the Inventory of Interpersonal Problems. Journal of Personality Assessment 55:521-536, 1990Crossref, Medline, Google Scholar
24. Diagnostic and Statistical Manual of Mental Disorders, 4th ed. Washington, DC, American Psychiatric Association, 1994Google Scholar
25. Spitzer RL, Williams JBW, Gibbon M: Structural Clinical Interview for DSM-III-R, Patient Version (SCID-P). New York, New York State Psychiatric Institute, Biometric Research, 1988Google Scholar
26. Cohen J: Statistical Power Analysis for the Behavioral Sciences, 2nd ed. Hillsday, NJ, Lawrence Erlbaum Associates, 1988Google Scholar
27. Gunderson JG, Frank AF, Ronningstarn EF, et al: Early discontinuance of borderline patients from psychotherapy. Journal of Nervous and Mental Disease 177:38-42, 1989Crossref, Medline, Google Scholar
28. Derogatis LR: SCL-90 Administration, Scoring, and Procedures Manual, I. Baltimore, John Hopkins University Press, 1977Google Scholar
29. Friis S, Wilberg T, Dammen T, et al: Pharmacotherapy for patients with personality disorders, in Treatment of Personality Disorders. Edited by Derksen J, Maffei C, Groen H. New York, Plenum, in pressGoogle Scholar



