Employee Assistance Programs in Private Health Plans: What Do They Offer?
Employee assistance programs (EAPs) address issues affecting work performance and well-being. Studies show positive EAP outcomes, although methodological limitations necessitate additional research (1). Health plans are among the vendors selling EAPs to employers, but data on these EAPs are sparse. Data are from a 2010 survey of private health plans in 60 markets. A total of 389 market area–specific plans (89% response) reported on behavioral health services in 939 insurance products. The analysis included 200 products (from 72 plans) reporting EAPs.
Most products (57%) required that purchasers pay additional fees rather than including the EAP without charge in standard packages (Figure 1). Only 12% of products contracted with an EAP vendor outside the plan. Although 36% recommended that enrollees use the EAP before accessing behavioral health benefits, only 4% required this. Forty-five percent of products with EAPs covered clinical assessment. Nearly all covered in-person and telephone counseling. All products reporting per-year limits reported eight-session limits. Of products with per-problem limits, 78% had a five-session limit, and the remainder had a six-session limit.
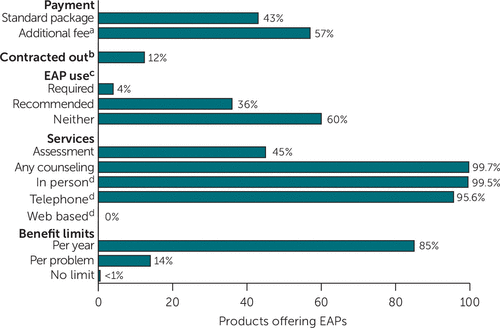
FIGURE 1 Features of private health plans’ employee assistance programs (EAPs) offered as part of health insurance products, 2010a
aDenominators for calculating percentages (weighted) were the number of products with nonmissing data; <2% of data were missing for all variables except EAP benefit limits (32.9% missing data).
bEAP vendor external to health plan
cBefore accessing behavioral health benefits
dCounseling modality
Study limitations included the focus on assessment and counseling; not all services were examined. Also, EAPs not viewed by plans as part of insurance products were excluded.
These health plan EAPs typically offered assessment and short-term counseling. Stakeholders concerned with differences between “free” and separately purchased EAPs will be interested that many EAPs are included in standard packages (2). The generally optional nature of EAPs aligns with federal regulations for the Mental Health Parity and Addiction Equity Act; an EAP cannot be a required gateway to behavioral health care unless it is also required for general medical services. Quantitative EAP limits are also consistent with parity. At least through 2014, EAPs are not subject to parity unless they provide “significant benefits in the nature of medical care or treatment.” Proposed excepted-benefits regulations would extend this exception and add other criteria.
1 : Revisiting employee assistance programs and substance use problems in the workplace: key issues and a research agenda. Psychiatric Services 58:1262–1264, 2007Link, Google Scholar
2 : The perceived value of “free” versus fee-based employee assistance programs. World at Work Journal 18:21–31, 2009Google Scholar



